Diabetes and the body (Diabetes UK video)


You might find it helpful to watch the animated video about diabetes and the body at the top of the page.
Type 2 diabetes is a lifelong condition where the level of glucose in the blood is too high. This happens because of a combination of 2 factors.
Insulin resistance
The pancreas is producing insulin but it cannot work properly because the body if 'resistant' to it. This means the body needs more and more insulin to achieve the same effect.
Insulin resistance is more likely in people:
Reduced insulin production
After a period of producing more and more insulin, the pancreas becomes exhausted and cannot make enough insulin.
Glucose is the main source of energy in our bodies. It is mostly made when our bodies break down the carbohydrates that we eat or drink.
Glucose is absorbed from the gut into the blood stream.
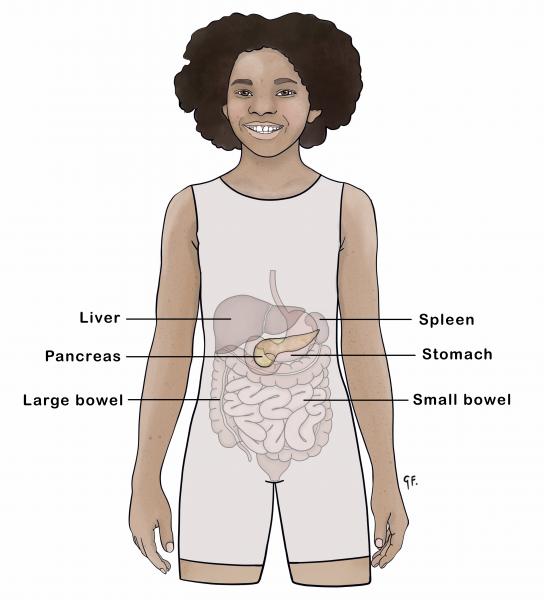
Insulin is a hormone produced by special cells called beta cells in the pancreas. The pancreas is an organ in the abdomen, behind the stomach.
Insulin allows the glucose from the bloodstream to move to the cells in the body. From there it's used as fuel for energy.
There are known risk factors for having type 2 diabetes.
You are more likely to develop type 2 diabetes if other members of your whānau have type 2 diabetes.
You can prevent or delay type 2 diabetes by making changes to the environmental risk factors.
The risk of getting type 2 diabetes lessens by becoming physically active and eating a healthy diet.
Type 2 diabetes is a lifelong condition. But the symptoms may lessen and the treatment may reduce if a person:
Symptoms usually develop gradually.
Some people with type 2 diabetes have few or no symptoms but a lot of tamariki and rangatahi will have the following symptoms:
If you suspect your child has diabetes, please seek medical attention as soon as possible.
Diabetes is diagnosed by assessing the risk factors and symptoms, and doing a blood test. If your child has risk factors for type 2 diabetes, your doctor may want to do blood tests for diabetes even when there are few symptoms.
Your child might need a test called an oral glucose tolerance test. This involves drinking a sweet liquid, and then checking glucose levels in the blood.
The goal of the treatment for type 2 diabates is to stabilise blood glucose levels as much as possible. The aim of treatment is to make your child feel better and to prevent health complications later in life.
The treatment of type 2 diabetes is about a balance between:
It's very important to involve all the family and whānau in supporting your child or young person to make healthy changes.
They can do this by:
See the KidsHealth page on healthy eating for children with diabetes [2].
All tamariki and rangatahi should aim to get 60 minutes of moderate to vigorous activity every day. This should include muscle-strengthening exercises 3 days a week.
See the KidsHealth page on encouraging children and young people with diabetes to be active [3].
If your child is using insulin, they may need to do the following around activity, to avoid hypoglycaemia:
Your diabetes team will discuss this with you.
Aim to limit recreational screen time to a maximum of 2 hours a day. Avoid things that involve sitting for long periods of time.
Please talk with your diabetes team about specific recommendations for your child.
Achieving and maintaining a healthy weight is an important part of diabetes management. It helps prevent health problems later in life.
Check further down the page for some resources to help you with healthy choices.
Most tamariki with type 2 diabetes need medicines:
Some tamariki may also need medicines to help with blood pressure, kidney health or cholesterol level.
It's important to monitor blood glucose levels and try to keep them within target range (4 to 8 mmol/L) even if your child is feeling 'OK' at the moment.
High blood glucose levels over a long period of time leads to serious complications. Screening is important to find any possible developing complications early.
Possible complications include:
Tamariki with type 2 diabetes and obesity are also at a higher risk of:
See KidsHealth's page on possible complications in children with diabetes [4].
You can minimise long-term risks and complications by:
There is a lot to learn about how to care for a child or young person with diabetes.
This learning involves the whole family, whānau, and other people that are involved in the life of a child or young person - school staff, friends, neighbours, sports coaches, etc.
A child or young person living with diabetes needs a lot of care and help with establishing healthy habits.
It's important that the whole family embrace and encourage healthy habit changes including:
Be supportive and understanding but make sure your child gets the treatment they need.
Help your child maintain long-term health and minimise the risk of diabetes complications.
Go to regular reviews by the diabetes team.
Talk to your child's school about extra supports that the school and the Ministry of Education can provide.
See KidsHealth's page about creating a safe environment for children with diabetes at school [5].
For example:
Tinana ora mо̄ ngā tamariki | Physical wellbeing for children resource [8]
Be smarter tool [9]
The content on this page has been approved by the Clinical Network for Children and Young People with Diabetes, Paediatric Society of New Zealand.
This page last reviewed 08 December 2023.
Email us [19] your feedback
Links
[1] https://www.kidshealth.org.nz/type-2-diabetes-children-general-guidelines-nutritional-management
[2] https://www.kidshealth.org.nz/healthy-eating-children-diabetes
[3] https://www.kidshealth.org.nz/encouraging-children-young-people-diabetes-be-active
[4] https://www.kidshealth.org.nz/possible-complications-children-diabetes
[5] https://www.kidshealth.org.nz/creating-safe-environment-children-diabetes-school
[6] http://www.diabetes.org.nz/
[7] http://www.diabetesfoundationaotearoa.nz/
[8] https://www.kidshealth.org.nz/sites/kidshealth/files/pdfs/Tinana-Ora-Mo-Nga-Tamariki.pdf
[9] https://www.kidshealth.org.nz/sites/kidshealth/files/pdfs/Bodywise-Be-Smarter-tool.pdf
[10] https://www.kidshealth.org.nz/tags/diabetes
[11] https://starship.org.nz/diabetes-resources/
[12] https://kidshealth.schn.health.nsw.gov.au/caring-diabetes-children-and-adolescents-4th-edition-2021
[13] https://diabetes.org/
[14] https://www.ispad.org/page/ISPADGuidelines2022
[15] https://onlinelibrary.wiley.com/doi/full/10.5694/mja2.50666
[16] https://www.kidshealth.org.nz/node/1865?language=ton
[17] https://www.diabetes.org.nz/youth
[18] https://www.diabetes.org.nz/branches/
[19] https://www.kidshealth.org.nz/contact?from=http%3A%2F%2Fwww.kidshealth.org.nz%2Fprint%2F2858%3Flanguage%3Dton