Appendicitis
Appendicitis
Appendicitis can be serious. Go first to your family doctor or after-hours medical centre if you think your child has symptoms of appendicitis. If you cannot get an appointment straight away, go to your hospital's accident and emergency department.
Key points about appendicitis
- the appendix is a small finger-like tube attached to the first part of the large intestine
- appendicitis is an inflammation of the appendix
- appendicitis is a potentially serious condition
- tamariki (children), especially those under 5 years old with appendicitis, can become unwell quickly
- go to your family doctor or after-hours medical centre first if you think your child has symptoms of appendicitis
- if you cannot get an appointment straight away, go to your hospital's accident and emergency department
What is appendicitis?
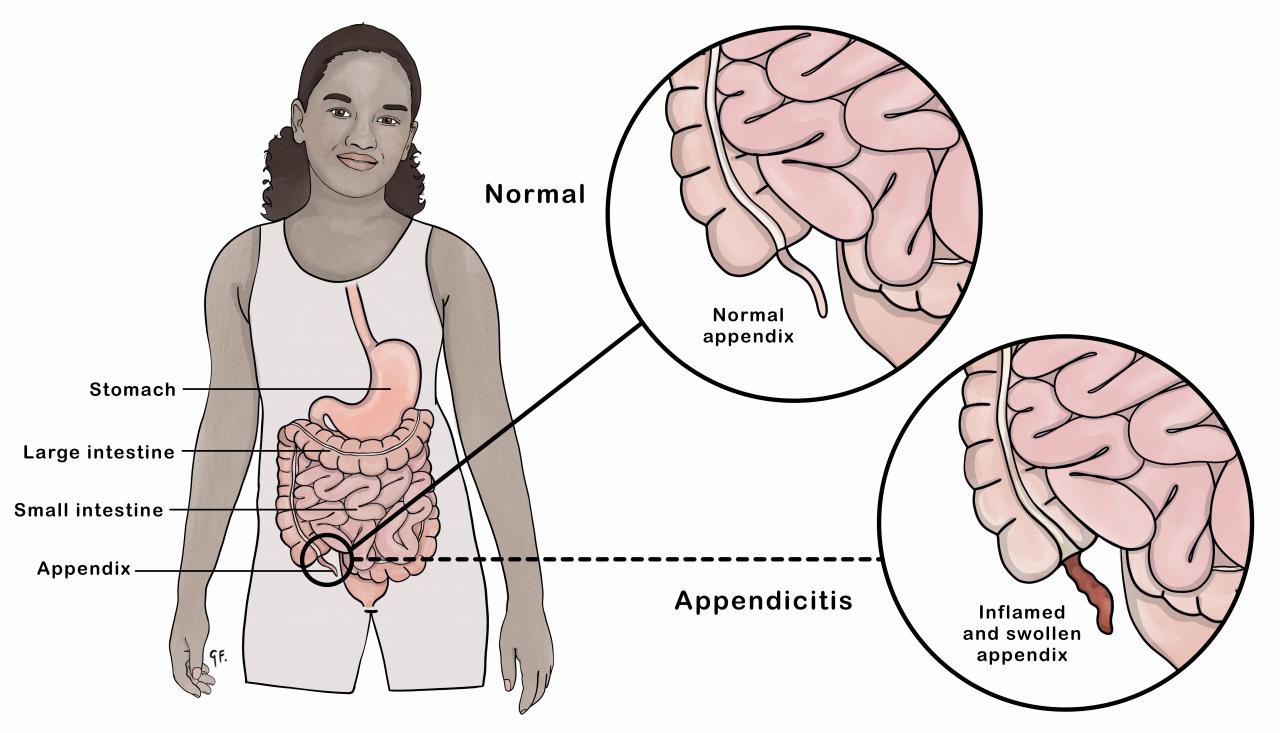
Appendicitis is when the appendix becomes inflamed and swollen. The appendix is a small finger-like tube that is attached to the first part of the large intestine (called the caecum). It is normally in the lower right side of the abdomen.
What causes appendicitis?
The appendix may become inflamed because of a blockage within it. The blockage causes the appendix to swell, and it can easily become infected by bacteria. Often, the cause is not clear.
What puts my child at risk of getting appendicitis?
Anyone can get appendicitis, but it occurs most often between the ages of 10 and 30. There is some evidence that the risk of appendicitis increases when there is not enough fibre in the diet.
What are the signs and symptoms of appendicitis?
Symptoms vary in different tamariki. The most common early symptom is continuous tummy pain around the belly button (navel). The pain may move to the lower right side of the tummy (abdomen) and become sharper and more severe. It often hurts more when your child moves around, and the pain worsens when coughing or walking.
Your child may also have:
- fever
- loss of appetite
- nausea (feeling sick)
- vomiting
- constipation or diarrhoea
How is appendicitis diagnosed?
A doctor can usually make a diagnosis of appendicitis after talking to you about your child's symptoms and by examining your child. Occasionally, a doctor may need to examine your child several times over several hours or even repeatedly over a day or two. Appendicitis can sometimes be difficult to diagnose, especially in younger tamariki.
In some circumstances, your child may need other tests, such as:
- an ultrasound scan
- blood tests
- a urine sample (to rule out a urinary tract infection)
See the KidsHealth section on x-rays and scans to learn more about different scans
When should I seek help for appendicitis?
Go first to your family doctor or after-hours medical centre if your child has symptoms you think may be due to appendicitis. If you cannot get an appointment straight away, go to your hospital's accident and emergency department.
Appendicitis can be a serious condition.
Do not give your child anything to eat or drink until the doctor has examined your child. This is in case surgery is needed.
You may give your child paracetamol to help reduce the pain. Follow the dosage instructions on the bottle. It is dangerous to give more than the recommended dose.
What are the complications of appendicitis?
If an inflamed appendix isn't removed by the surgeon, it can sometimes burst. If this happens, the infected contents of the appendix spill into the abdominal cavity. This is a more serious medical emergency. If left untreated, it can lead to an infection of the lining of the abdominal cavity (peritonitis), which can be life-threatening. This requires emergency treatment, including an intravenous line (IV) and antibiotics.
The signs of a perforated appendix include:
- a severe worsening of symptoms - especially severe and constant tummy pain
- not wanting to move because it makes the pain worse
What is the treatment for appendicitis?
Usually, an operation called an appendicectomy is done to remove the appendix.
In some specific situations, surgery may be put off while your child is treated with antibiotics.
There are 2 ways this surgery can be done - an open appendicectomy and a laparoscopic appendicectomy.
Open appendicectomy
A surgeon makes a single cut (incision) over where the appendix is. The inflamed appendix is removed through this cut.
Laparoscopic appendicectomy ('keyhole' surgery)
A surgeon will make 3 small 'keyhole' cuts over the lower abdomen. Then, they insert special instruments through these cuts to remove the appendix.
When a laparoscopic appendicectomy becomes an open appendicectomy
Sometimes, a laparoscopic appendicectomy may need to become an open appendicectomy if the surgeon cannot safely remove the appendix any other way.
Your child will have the surgery under general anaesthetic (GA) - they will be completely asleep.
See the KidsHealth page on anaesthetic to learn more about what a GA involves
Discussing the operation with the surgical team
Your child's surgical team will discuss your child's operation with you, including which technique they will use. You can ask them any questions you have then.
When the surgeon finds something else during the appendicectomy
Occasionally, a surgeon will find another cause for the pain during the appendicectomy. If this happens, the surgeon will deal with it during the same operation.
When your child needs IV antibiotics
All children having an appendicectomy will get at least one dose of antibiotics during the surgery.
Sometimes, if your child's symptoms have been going on for many days or if it is an advanced or complex case, doctors will give strong antibiotics through an intravenous (IV) drip. If this happens, your child's doctor may delay the surgery deliberately.
See the KidsHealth page on drips to learn more about IV drips
What happens to my child before the operation to remove their appendix?
- your child will not be allowed to eat or drink anything
- your child will need to have an intravenous (IV) drip put into their hand or arm before the operation
- your child's surgeon will explain the operation and any other treatment needed - you should feel free to ask the surgeon any questions you have
- your child will receive antibiotics at the time of surgery
- you will need to sign a consent form before the surgery
In some cases, your child may need a nasogastric tube - a tube through the nose to the stomach. Your child is more likely to need this if their appendicitis has been going on for a long time or they have vomited a lot.
What happens to my child after the operation to remove their appendix?
- the healthcare team will watch your child closely immediately after the operation and as often as necessary
- they will check the wound regularly
- the nurses on the ward will give your child pain relief
- older children may be able to control their own pain relief through something called 'patient controlled analgesia (PCA)'
- your child may have antibiotics through an intravenous (IV) drip for several days after the surgery if the appendix bursts or there is peritonitis
- your child's hospital stay will usually be between 1 and 4 days but may be longer if the appendix bursts or there is peritonitis
See the KidsHealth section on pain management to learn more about different types of pain relief
Can there be any complications from the operation to remove my child's appendix?
All surgery comes with some potential risks. One of the most common complications following appendicectomy is infection. Around 20% of people with a burst appendix develop an abscess (collection of pus) inside their tummy. This usually shows up within 2 weeks after the appendicectomy.
If an abscess does develop, your child may need another operation to drain it. Often, doctors can use a special x-ray to help guide them as they insert a narrow tube to drain the pus. Your child won't need a full operation if doctors use this technique.
This page last reviewed 11 September 2023.
Do you have any feedback for KidsHealth?
If you have any feedback about the KidsHealth website, or have a suggestion for new content, please get in touch with us.
Email us now