Asthma
Asthma
Asthma is a condition that leads to narrowing of the airways of the lungs. Symptoms include wheeze, cough and difficulty breathing.
Key points about asthma
- asthma is a condition that leads to narrowing of the airways of the lungs
- symptoms include wheeze, cough and difficulty breathing
- common asthma triggers are colds (viruses), exercise, dust, pollens and cigarette smoke
What is asthma?
Asthma is a common breathing condition. It affects the small and medium-sized airways (bronchi) in the lungs.
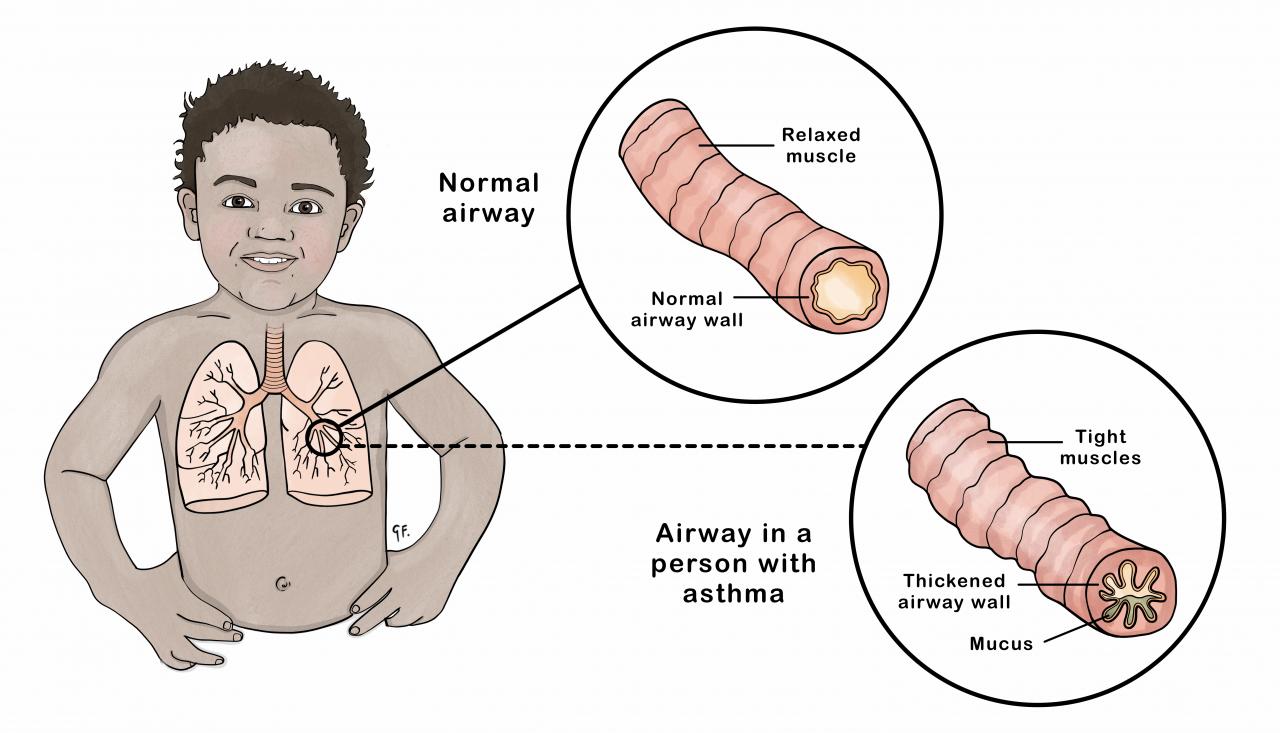
In asthma, your child's airways are inflamed and there is:
- swelling of the airway wall
- an increase in mucus or phlegm
- tightening of the muscle in the airway wall (see the image at the top of the page)
These changes cause narrowing of your child's airways. This leads to wheezing, cough and difficulty with breathing.
Wheezing is a musical, whistly sound that tamariki make, usually when breathing out. It can also happen when they breathe in. The sound comes from the chest, not from the nose or throat.
Why do some children have asthma?
One in 4 tamariki in New Zealand will have asthma at some time during childhood.
It is not clear why some tamariki have asthma when others do not.
Asthma in tamariki is more likely if:
- a mother smoked during pregnancy
- a child has eczema, hay fever or allergies
- there is asthma in the family - parent, brother or sister
- one or both parents have an allergic condition such as asthma, hay fever or eczema
Modern Western lifestyle may play a part in the rise in asthma that has happened over the last few decades. Changes in housing, diet and a more hygienic environment may contribute. Outdoor environmental pollution may make asthma symptoms worse but it does not actually cause asthma. Experts continue to study the reasons for the increase in asthma.
What causes an asthma attack?
Tamariki and rangatahi with asthma have airways that are sensitive and react to certain triggers.
Some tamariki have asthma all year round. Others may only have it in certain seasons or situations.
Infections
Viruses like colds and the flu can cause some tamariki to have worse asthma symptoms which may lead to an asthma attack.
Allergies
If your child is allergic to things like pollens, grass, dust or pet fur, this can worsen their asthma.
Irritants
Irritants may trigger asthma attacks. Examples or irritants are air pollution, car exhaust, vapours and mouldy environments.
Tobacco smoke
Tobacco smoke can trigger asthma attacks and can make your child's asthma symptoms worse. All tamariki need a smoke-free environment, wherever they happen to be.
Exercise
Exercise and physical activity are a big part of helping tamariki stay healthy and fit. Exercise is also an important part of asthma management. But, sometimes exercise or activity can trigger an episode of asthma.
Changes in the weather
Some tamariki may find a change in the weather or certain conditions, like cold or damp weather, can make their asthma worse.
How can I prevent my child from having asthma attacks?
Some tamariki need to be on a preventer medicine.
See the KidsHealth page on the different types of asthma medicines and when to use them.
Other things that can help your child's asthma include:
- living in a smoke-free environment at all times
- keeping your house warm and dry
- where possible, avoiding things that trigger their asthma
Making sure your child's environment is smoke-free
Make sure your child's environment is smoke-free, wherever they happen to be. Asthma increases in tamariki whose parents smoke. Tobacco smoke also triggers asthma attacks and makes a child's asthma more severe. Many environmental factors contribute to asthma. Cigarette smoke is one that you can avoid.
If you want to give up smoking:
- call the free Quitline on 0800 778 778 or text 4006
- check out the Quitline | Me Mutu website
- ask your healthcare provider for support
Keeping your house warm and dry
Check out some tips for keeping your home warm and dry.
Keep a symptom diary and a record of possible triggers
Asthma symptoms and triggers may differ from child to child and from time to time. It is useful to know your child's triggers. Keep a symptom diary and keep a record of possible triggers.
Could my child have asthma?
See your doctor and ask about asthma if your child:
- wheezes and coughs with a cold (virus)
- wheezes and coughs after exercise
- wheezes and coughs during the night
- cannot keep up when they are running around with tamariki of the same age
- says they are out of breath or breathless
- complains they feel tired or ask you to carry them (depending on their age) when you go for a walk
- does not run around as much as tamariki of the same age
These are some of the symptoms of asthma in tamariki. But, these symptoms may be due to other less common conditions. Talk to your doctor.
What if my child does have asthma?
Asthma medicines
Find about about the different types of medicines to treat asthma in tamariki.
Online learning tool
You can use the Asthma + Respiratory Foundation NZ's online learning tool to learn more about how you can help tamariki with asthma stay fit, healthy and happy.
Booklets to download
You can read the following translated booklets alongside the online learning tool above.
Read a booklet about managing your child's asthma in te reo Māori (PDF, 3.06 MB)
Read a booklet about managing your child's asthma in English (PDF, 3.59 MB)
Read a booklet about managing your child's asthma in Samoan (PDF, 3.05 MB)
Videos to watch
Watch some videos about managing asthma in children and young people.
How do I treat my child's asthma attack?
Find out about mild, moderate and severe asthma attacks and what to do if your child has one.
Will my child grow out of asthma?
Asthma is a long-term condition. The majority of tamariki with asthma have less troublesome asthma as teenagers. Symptoms can appear again in adulthood. If your child has severe asthma, it is more likely to continue or return in later life.
Your child should learn about asthma and gradually take over responsibility for its management, as they become a teenager, with support from you.
See more KidsHealth content on asthma
This page last reviewed 10 July 2023.
Do you have any feedback for KidsHealth?
If you have any feedback about the KidsHealth website, or have a suggestion for new content, please get in touch with us.
Email us now