Croup
Croup
Croup is a viral illness in young children which causes narrowing of the upper airways. Croup is often a mild illness but can quickly become serious, so don't hesitate to get medical help.
Key points about croup
- croup is a viral illness in young children which causes narrowing of the upper airways
- croup is often worse at night
- croup is often a mild illness but can quickly become serious, so do not hesitate to get medical help
- if your child has stridor (a harsh noise heard when breathing in) while they are calm and not upset, take them to your doctor or the nearest hospital straightaway
- if there is severe breathing difficulty or distress, or your child becomes blue, pale or drowsy, dial 111 within New Zealand for urgent medical help (use the appropriate emergency number in other countries)
- there is effective treatment for severe episodes of croup
- steam doesn't help and may lead to accidental burns - do not use it
What is croup?
Croup is a viral illness in young children, which causes narrowing of the upper airways. Some children have recurring croup and this may need further assessment.
How does croup develop?
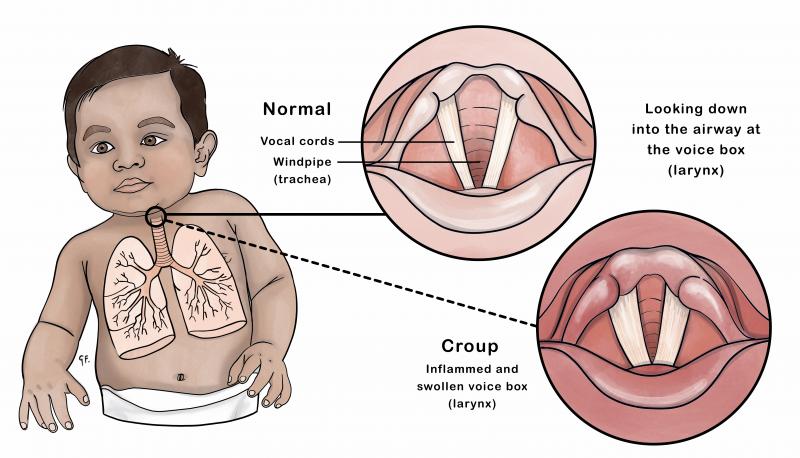
When you breathe, air passes through the voice box (larynx) and windpipe (trachea) into the lungs. In croup, a viral infection causes inflammation and swelling of the lining of the voice box and windpipe, which become narrowed. When the airway becomes narrowed, breathing in becomes more difficult, and you can hear stridor (a harsh noise when breathing in).
Who gets croup?
Toddlers are most likely to get croup.
Toddlers are most likely to get croup. Their windpipes are softer than those of older children. When the airways become inflamed, they narrow and this causes stridor. If your child gets croup and is less than 6 months of age, or of school age, you should discuss it with your family doctor.
What are the signs and symptoms of croup?
The major features are:
- a cough which is harsh and often described as 'barking'
- stridor (noisy breathing, with a harsh sound heard as your child breathes in)
Stridor may only last for a few days while the cough may last for up to a week or so. Your child's voice is usually hoarse. Breathing becomes more difficult and the stridor worsens when your child becomes upset.
The symptoms of croup seem to often appear or worsen at night. Before the cough and breathing trouble develop, your child may have other signs of the viral illness such as:
- a sore throat
- a temperature
- red eyes
- a runny nose, or
- a poor appetite
Check out the signs that your child is struggling to breathe
What is the treatment for croup?
Viruses cause croup, so antibiotics do not help.
Mild croup
If your child has a mild case of croup, then you can manage it at home without medicine.
Moderate to severe croup
In moderate to severe croup, doctors may prescribe steroid medicine. This reduces the swelling in your child's airway and helps them to breathe more easily. It does not change the cough but does reduce the stridor (the harsh noise heard when your child breathes in) which is the most serious aspect of the illness. Steroids work for about 48 hours.
In the most severe cases, your child may need to have nebulised adrenaline in hospital.
How can I care for my child with croup at home?
Calming and comforting your child
If you are caring for your child with mild croup at home and they become upset, try to calm and comfort your child on your lap. Distress can worsen the breathing difficulty and stridor.
Helping with a sore throat or fever
Cool sips of fluid may be soothing if your child's throat is sore.
You can give paracetamol if your child is miserable with a fever or has a sore throat. You must follow the dosage instructions on the bottle. It is dangerous to give more than the recommended dose.
Go to the doctor if croup gets worse
If their croup gets worse and you are worried that it might be serious, take your child to their doctor, the nearest accident and emergency clinic or the nearest hospital emergency department for help
Don't use steam
Although adding steam to the air (humidification) used to be recommended, there is no evidence it actually helps, and there have been several cases reported where children have been badly burned from the hot water. For these reasons, doctors do not recommend using steam for croup.
How long does croup last?
Croup is usually at its worst in the first few days of the illness.
Generally, croup is at its worst in the first few days of the illness. Stridor may only last for a few days while the cough may last for up to a week or so.
When should I seek help for my child with croup?
When do I need to see a doctor urgently?
If your child has any of the following, go to a doctor or the nearest hospital straightaway:
- there is stridor (a harsh noise heard when breathing in) when your child is calm and not upset
- you are worried your child is having increasing difficulty with their breathing
- your child becomes persistently upset and can't be consoled
- your child has additional signs of ill health (such as pale colour, a very high temperature, cool or clammy hands and feet, or dribbling)
- you become concerned for any other reason
Check out the signs that your child is struggling to breathe
When should I dial 111?
Dial 111 within New Zealand (use the appropriate emergency number in other countries) and ask for urgent medical help if your child has any of the following:
- becomes blue
- becomes pale or blue after a coughing spell
- has extreme difficulty breathing
- there is a change in their behaviour (for example, they become drowsy, agitated or delirious)
- has pauses in breathing
Could there be another reason for my child's croup-like symptoms?
In babies less than 6 months of age, or in children older than 6 years, croup is less common. There could be another reason for their symptoms. Make sure to take your child to your family doctor for a check up. Your child might need to see a paediatrician (a specialist in children's health) or ENT (ear, nose and throat) specialist.
What happens if my child gets croup again?
It is very uncommon for children to have more than one episode of croup a year for their first 2 or 3 years. Go to your family doctor and ask for a review of your child's symptoms if they have continuing symptoms of either:
- stridor
- barking cough (that is, several episodes each year, or episodes that continue into school age)
Your child may need to see a paediatrician (specialist in children's health) or ENT (ear, nose and throat) specialist.
This page last reviewed 07 December 2021.
Do you have any feedback for KidsHealth?
If you have any feedback about the KidsHealth website, or have a suggestion for new content, please get in touch with us.
Email us now