Key points about children's pain
- as parents, you are often the best judge of your child's pain
- listen to what your child is telling you and watch how they're behaving
- if you have worries about your child's pain, talk to a health professional
- if you're not sure about giving your child medicine for pain, ask a health professional for advice
What is pain?
Young tamariki (children), or tamariki who are unwell, cannot always explain what they are feeling. This can be upsetting for parents and whānau, who may feel unsure about what their child is experiencing. Parents usually know their child’s normal behaviour, but pain or fear can change how a child reacts.
Things that can affect your child’s experience of pain include their:
- age
- understanding of what is causing the pain
- confidence in their ability to cope
- past experiences of pain and what they have seen others do
- learned responses to pain
Acute or chronic pain
Acute pain
Acute pain is short-term pain. An operation, injury, illness, or medical procedure can all cause pain. The pain may last from a few seconds (for example, a needle) to a few weeks or months (for example, after an injury).
Some pain after an operation is normal and part of healing. Medicine can help reduce acute pain. You can also support your child by using methods such as relaxation and distraction.
Chronic or persistent pain
Chronic or persistent pain lasts longer, usually more than 3 months. The pain may be constant or it may come and go.
It can be hard to find a cause for persistent pain. Treatments and support programmes can help your child manage this type of pain.
See the page on chronic or persistent pain to learn more.
Chronic Or Persistent Pain In Children & Young People
Knowing if your child is in pain
It is not always easy to know how much pain your child is in. Listening to what they say and watching what they do can help give you a better idea.
Signs your child may be in pain include:
- crying
- facial changes or pulling a face such as a grimace or frown
- changes in sleeping or eating patterns
- becoming quiet or withdrawn
- screaming
- refusing to move
- changes in how they usually function
Remember, these changes can also happen when a child feels scared or frightened. Some tamariki may say they are sore but find it hard to explain how much it hurts.
There are tools that can help with this.
Faces pain scale
The faces pain scale asks your child to point to a face that shows how much pain they feel, from ‘no pain’ to ‘very much pain’. You can tell staff which face your child chose. This helps them understand how your child is feeling.
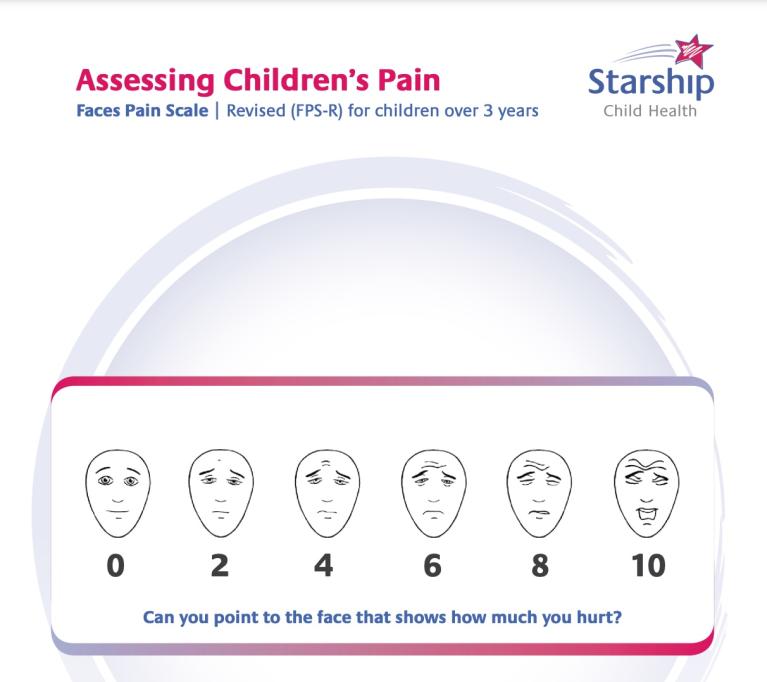
Source: Starship
Modified pain rating scale
There is another tool to assess pain in young tamariki or those with a developmental disability. For each category, choose a score of 0, 1 or 2 and add them together to get a total out of 10. This score can help you explain your child’s pain to staff.
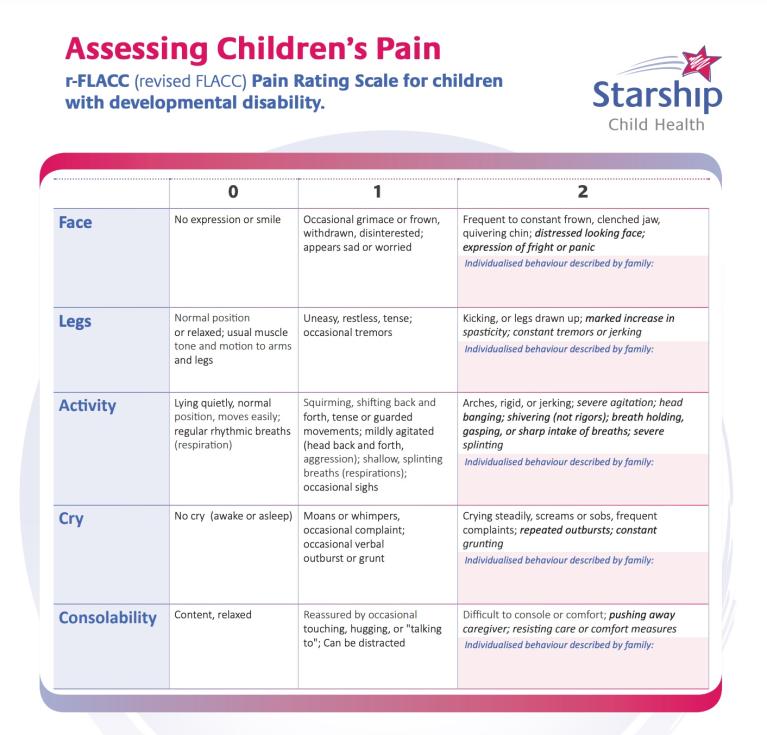
Source: Starship
More information

Visit the Centre for Pediatric Pain Research website for helpful information about children’s pain and how to better understand and manage it.
Acknowledgements
Starship Foundation and the Paediatric Society of New Zealand acknowledge the cooperation of The Children's Hospital at Westmead, Sydney Children's Hospital at Randwick, and Kaleidoscope - Hunter Children's Health Network in making this content available to patients and families.
