What is an IV line?
An IV line is sometimes known as a cannula.
It's a short, small plastic tube with a needle inside.
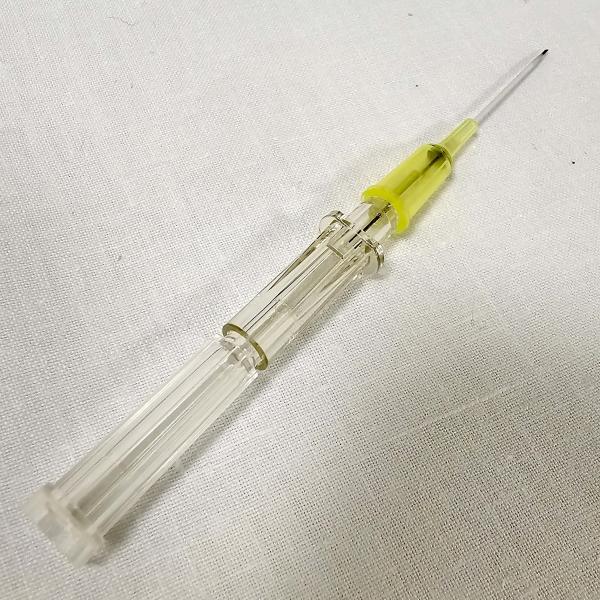
An IV cannula with the needle still attached to the cannula.
A member of the healthcare team will put the IV line into your child's vein.
They will take the needle out and leave the plastic tube in so they can use medicines to treat your child.
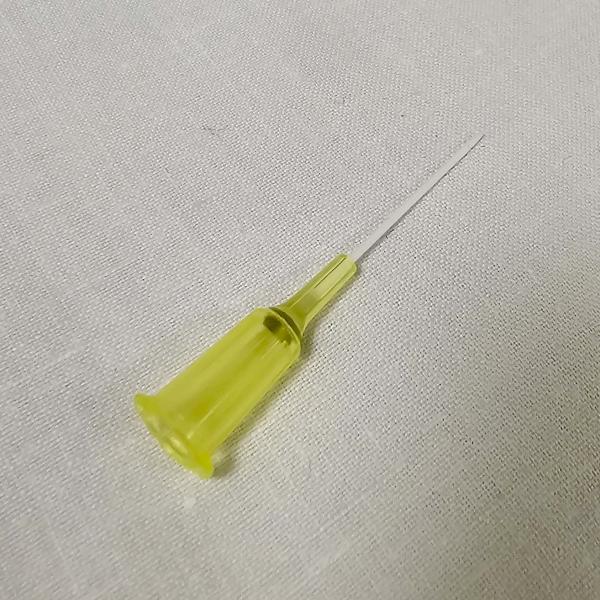
An IV cannula with the needle removed.
Sometimes, a doctor or nurse may take blood samples from the IV line.
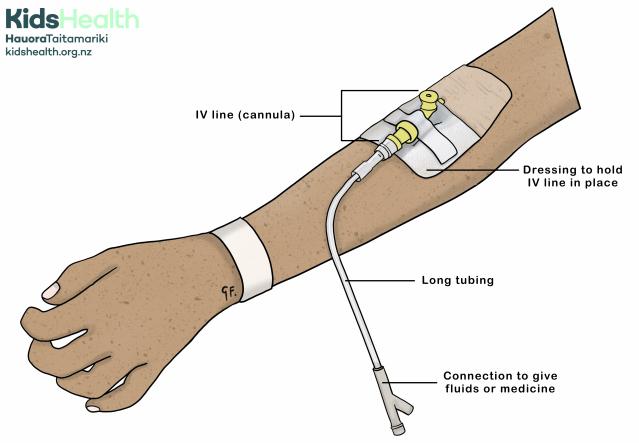
An illustration of an IV line (cannula) in place on the arm.
Source: KidsHealth
transcribeTranscript
The illustration shows an arm with an intravenous (IV) line inserted in the arm.
- A transparent dressing secures the IV line in place.
- A label points to the IV line (cannula), which is a small tube placed into a vein.
- Another label points to the dressing to hold IV line in place, which keeps it secure.
- The long tubing extends from the IV line and connects to a port labelled connection to give fluids or medicine.
- At the wrist is a white wristband.
At the top left of the illustration is the KidsHealth logo with the website: kidshealth.org.nz
Reasons for needing an IV line
The IV line will allow your child's medicine to go directly into their vein.
Your child will have an IV line if they are too sick to swallow medicine or if it is the best way to give medicine.
How IV lines are put in
The doctor or nurse may first put a numbing cream on your child’s skin. It takes about 30 to 60 minutes for the numbing cream to work. If your child needs an IV line urgently, there may not be time to put on numbing cream.
A doctor or nurse will use a tight band (tourniquet) around your child's arm or leg.
Your child will need to be still while the IV line is put into their vein. The healthcare team will help you comfort and hold your child.
Once the IV line is in the vein, the doctor or nurse will take out the needle, leaving the plastic tube in. Tape and bandages will hold the plastic tube in place.
Your child may have a padded board (splint) to keep their hand or foot still.
The doctor or nurse may take blood tests from the IV line when they are putting it in. If they cannot collect enough blood from the IV line, your child may need a separate blood test.
How your child will receive medicine
A doctor or nurse will attach long tubing or syringes to the IV line to give the medicine. Often, the doctor or nurse will put long tubing into a special (IV) pump. It controls the amount of medicine that will go in.
Your child's healthcare team will discuss with you how long the IV line needs to stay in. This will depend on why your child is having the IV line, and how quickly they get better.
Possible problems with IV lines
IV lines can block, leak or become infected. The healthcare team will regularly check the IV line and the area around it. They will look for redness, swelling, leakage and pain where the IV line goes in. Sometimes, they may need to put a new IV line in another place. There can be a bruise around where the IV line was. This will soon fade.
If you are worried, please ask the healthcare team to check your child's IV line.
Supporting your child while they have an IV line put in
You can comfort your child by staying with them as the IV line is put in.
It is helpful to distract your child by cuddling, telling stories, singing or playing with a toy or game. Try to remain calm and comfort your child. Praise your child afterwards - putting in an IV line is not easy for a child.
The staff are there to help you and your child. If you would like more information, please ask the healthcare team caring for your child.
Acknowledgements
Illustration of child's arm with a cannula in place by Dr Greta File. Property of KidsHealth.
Photos of cannula with and without needle property of KidsHealth.
References
IV - the facts about drips | The Sydney Children's Hospitals Network.
