Ear infections animation
An animation about ear infections, including symptoms and when to see a health professional.
Source: KidsHealth
transcribeTranscript
Ear infections are very common in young tamariki.
They can cause fever and ear pain.
Viruses or bacteria cause ear infections.
They often happen at the same time as a cold.
An ear infection usually affects the area behind the eardrum.
Tamariki with an ear infection may:
- have a fever
- be 'clingy' and 'grizzly'
- not drink or feed as much as usual
- have ear pain or start tugging at their ear
- have fluid leaking from their ear
- get more upset when they lie down
- be more unsteady on their feet
If you think your child has an ear infection, see a health professional.
They can look in your child’s ear and see if there are signs of infection.
Ear infections do not usually need treatment with antibiotics.
Regular pain relief with paracetamol is important to help your child feel more comfortable.
Go back to a health professional if:
- an earache is not settling after 2 days or
- fluid starts coming out of your child's ear or
- your child seems more unwell or
- you are worried
Some tamariki can have thick fluid which stays stuck behind their eardrum.
This is called glue ear which can affect hearing and speech development.
If you’re worried your child could have glue ear, always see a health professional.
Most children with an ear infection get completely better.
It is not easy to prevent ear infections, but the following may help reduce the risk:
- making sure your child's environment is smoke-free
- breastfeeding your baby
- keeping your child's room warm and dry
- making sure your child has their vaccinations on time
An animation about ear infections, including symptoms and when to see a health professional.
Source: KidsHealth
transcribeTranscript
E kitea noatia ngā pokenga taringa i te tamariki.
Ka puta pea he kirikā me te mamae.
He huaketo, he huakita rānei ngā pūtake o ngā pokenga taringa.
Puta ai aua mate i te nuinga o te wā i te wā tonu o te rewharewha.
I te nuinga o te wā ka pā mai te pokenga taringa ki te wāhi kei muri o te tōrino.
Ko ngā tamariki e pāngia ana e te pokenga taringa, tērā pea:
- ka kirikā
- ka kaha pīrangi kia awhitia, ka tangitangi hoki
- he iti iho te inu, te kai rānei i tō te nuinga o te wā
- ka rongo i te mamae taringa
- ka turuturu te wē mai i tōna taringa
- ka kaha ake te auhi ina takoto ia
- ka kaha ake te ruriruri o ngā waewae
Ki te whakaaro koe ka pāngia pea tō tamaiti e te pokenga taringa, toro atu ki tētahi ngaio hauora.
Ka tirotiro ia ki tō tāu tamaiti taringa kia mōhio ai mēnā he tohu pokenga i reira.
I te nuinga o te wā kāore ngā rongoā paturopi e hiahiatia ana hei maimoatanga mō ngā pokenga taringa.
He mea nui te auau o te kai rongoā pēhi mamae (arā, paracetamol) hei āwhina kia nui ake te hāneanea o tō tamaiti.
Hoki atu ki tētahi ngaio hauora mēnā:
- kāore anō kia tau haere te mamae taringa whai muri i te 2 rā, tērā rānei
- ka tīmata te putanga o te wē i tō tāu tamaiti taringa, tērā rānei
- ka kaha ake te māuiuitanga o tō tamaiti, tērā rānei
- kei te āwangawanga koe
Mō ētahi tamariki ka mau pea he wē kukū i muri i te tōrino.
E kīia ana tēnei he taringa hoi, tērā ka pā kino pea ki te whanaketanga o te rongo me te reo ā-waha.
Ki te āwangawanga koe kua pāngia pea tō tamaiti e te taringa hoi, toro atu i ngā wā katoa ki tētahi ngaio hauora.
Ko te nuinga o ngā tamariki e pāngia ana e te pokenga taringa, ka piki katoa te ora ki a rātou.
Ehara i te mea he māmā te ārai atu i ngā pokenga taringa, engari ka āwhina ko ēnei e whai ake ana hei whakaiti i te tūponotanga:
- te whakarite kia auahi-kore te whaitua o tō tamaiti
- te whāngote i tō pēpi
- te whakarite he mahana, he maroke hoki te rūma o tō tamaiti
- te whakarite kia whiwhi tō tamaiti i ngā rongoā āraimate hei te wā tika
An animation about ear infections, including symptoms and when to see a health professional.
Source: KidsHealth
transcribeTranscript
O tulaga masani le siamā o taliga o tamaiti laiti.
E oso ai le fiva ma le tiga o taliga.
E mafua mai siama.
O aafiaga e masani na oso pe a fulū.
E masani na aafia ai le puipui o le taliga pe a siamā le taliga.
O tulaga nei e ono vaaia i tamaiti ua siamā taliga:
- fiva
- ‘matanana’ ma le ‘fai aso’
- ua lē tutusa le inu po o le ‘ai
- tiga le taliga po o le tago falō lona taliga
- sau le sua mai le taliga
- fiu e faafilemu pe a faataoto
- tevateva pe a savali
Vaai se sui faalesoifua maloloina, pe a masalomia ua siamā le taliga.
E mafai na autilo i totonu o le taliga e iloa ai pe ua siamā.
E tele na lē moomia se fualaautui e togafitia ai le siamā o le taliga.
E taua le faainu sana paracetamol e faatea ai le tiga.
Toe vaai se tomai faalesoifua maloloina pe afai:
- ua 2 aso e lē te‘a le tiga o le taliga po o le
- amata na sau le sua mai lona taliga po o le
- tigaina si au tama po o lou
- popole foi
O nisi tamaiti e mafiafia le sua e to‘a i tua atu ma le puipui o le taliga.
E aafia ai lana faalogo ma le tautala pe a to‘a le sua i le taliga.
Ave e vaai se fomai, pe a e popole i le to‘a o le sua i lona taliga.
O le toatele o tamaiti e toe manuia mai le siamā o taliga.
E lē faigofie le puipuia mai le siamā o taliga, ae aoga gaioiga nei e tuuitiitia ai tulaga e lamatia ai:
- faamautinoa e lē o mānavaina e tamaiti asu sikaleti
- faasusu pepe i lou suasusu
- faamafanafana ma faamatū lelei lona potu
- faamautinoa ua fai ana tuipuipui i taimi faatulagaina e fai ai
An animation about ear infections, including symptoms and when to see a health professional.
Source: KidsHealth
transcribeTranscript
‘Oku hoko angamaheni ‘aupito ‘a e mahaki‘ia ‘a e telingá ‘i he fānau iikí.
Te nau lava ‘o fakatupunga ‘a e mofi mo e langa ‘a e telingá.
‘E lava ke fakatupunga ‘e he ngaahi vailasí pe pekitīliá ‘a e mahaki‘ia (infection) he telingá.
‘Oku nau fa‘a hoko ‘i he taimi tatau mo hano ma‘u ‘e he momokó.
‘Oku fa‘a uesia ‘e he mahaki‘ia ‘a e telingá ‘a e ‘ēlia ‘i mui ‘i he nafa ‘o e telingá (eardrum).
‘E malava ki he fānau ‘oku mahaki‘ia honau telingá ke:
- nau mofi
- ‘fakafiufiu (clingy)’ mo ‘tatangi (grizzly)’
- nau ta‘efiefie inu pe kai ‘o hangē ko e angamahení
- langa honau telingá pe kamata ke toutou ala ‘o fusi (tugging) honau telingá
- hafu honau telingá
- nau mamahi‘ia ange he taimi te nau tokoto ai ki laló
- ngā vaivai ange he taimi ‘oku nau tu‘u ‘aki ai honau va‘é
Kapau ‘okú ke fakakaukau ‘oku mahaki‘ia ‘a e telinga ‘o ho‘o tamá, sio leva ki ha tokotaha ngāue palofesinale ki he mo‘ui leleí.
Te nau sio ki loto ‘i he telinga ‘o ho‘o tamá ke vakai‘i pe ‘oku ‘i ai ha ngaahi faka‘ilonga ‘o ha mahaki‘ia.
‘Oku ‘ikai ke fa‘a fiema‘u ha ‘enitipaiotiki ia ke faito‘o ‘aki ‘a e mahaki‘ia ‘a e telingá.
‘Oku mahu‘inga ke hokohoko hono fakanonga ‘a e mamahí ‘aki ‘a e panatolo (paracetamol) ke tokoni ki hono fakafiemālie‘i ange ‘a ho‘o tamá.
Toe foki ki ha tokotaha ngāue palofesinale ki he mo‘ui leleí kapau:
- ‘oku ‘ikai faka‘au ke sai ha telinga ‘oku langa hili ha ‘aho ‘e 2 pe
- ‘oku kamata ke hafu e telinga o ho‘o tamá pe
- ‘oku faka‘au ke toe puke lahi ange ‘a ho‘o tamá pe
- ‘okú ke hoha‘a
‘Oku ‘i ai ‘a e fānau ‘e ni‘ihi ‘e lava ke ‘i ai ha huhu‘a matolu ‘oku nofo ‘o pipiki ‘i mui ‘i he nafa ‘o honau telingá.
‘Oku ui eni ko e telinga fonu te‘etuli (glue ear) ‘a ia te ne ala uesia ‘a e fanongó mo e fakalakalaka ‘a e leá.
Kapau ‘okú ke hoha‘a pe ‘oku ‘oku fonu te‘etuli ‘a e telinga ‘o ho‘o tamá, sio ma‘u pē ki ha tokotaha ngāue palofesinale ki he mo‘ui leleí.
Ko e tokolahi taha ‘o e fānau ‘oku mahaki‘ia honau telingá ‘e faka‘au pē ‘o sai ‘aupito.
‘Oku ‘ikai faingofua ‘a e faka‘ehi‘ehi mei he mahaki‘ia ‘o e telingá, ka ‘e tokoni ‘a e ngaahi me‘a ko ‘ení ki hono fakasi‘isi‘i ‘a ‘ene malava ke hokó (risk):
- ko hono fakapapau‘i ‘oku ‘ikai ke fakahoko ha ifi tapaka ‘i he ‘ātakai ‘o ho‘o tamá
- ko hono fakahuhu ‘a ho‘o pēpeé
- ko hono tauhi ke māfana mo mātu‘u ‘a e loki ‘o ho‘o tamá
- ko hono fakapapau‘i ‘oku fakahoko taimi totonu ‘a e ngaahi huhu malu‘i ‘a ho‘o tamá
Watch an animation on ear infections in your preferred language.
Key points to remember about ear infections
- ear infections are very common in young tamariki
- they can cause pain and fever
- if you think your child has an ear infection, take them to a health professional
- pain relief is important
- most tamariki outgrow ear infections and will have normal, undamaged ears and normal hearing
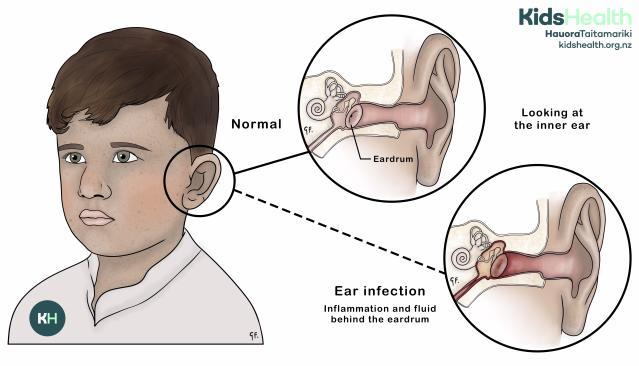
An illustration showing inflammation and fluid behind the eardrum during an ear infection.
Source: KidsHealth
transcribeTranscript
The illustration shows a young child from the shoulders up, with two close-up circles showing a side view of the inner ear.
- The top circle, labelled Normal, shows a healthy eardrum and clear middle ear space.
- The bottom circle, labelled Ear infection, shows inflammation and fluid behind the eardrum.
- A dashed line connects the circles to the child’s ear.
At the top right is the KidsHealth logo with the website: kidshealth.org.nz.
What the inside of the ear looks like
The inside of the ear has 3 parts - the outer, middle and inner ear.
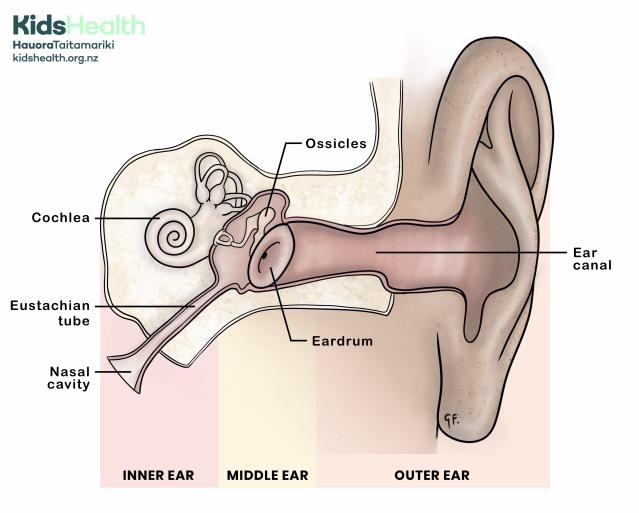
Illustration showing the anatomy of the ear including the inner, middle and outer ear.
Source: KidsHealth
transcribeTranscript
This ear anatomy illustration shows the main parts of the ear divided into the inner ear, middle ear and outer ear.
Labelled parts:
- Ear canal
- Eardrum
- Ossicles
- Cochlea
- Eustachian tube
- Nasal cavity
At the top left is the KidsHealth logo with the website: kidshealth.org.nz.
What is an ear infection?
Ear pain and concerns about hearing are some of the most common reasons parents take their young tamariki to a health professional. In tamariki, these things are often caused by problems in the middle ear.
There are 2 common types of middle ear problems.
An ear infection
Acute otitis media is the medical term for an ear infection. It is an infection behind the eardrum. The information on this page is about ear infections.
Glue Ear
Glue ear is also known as otitis media with effusion. Glue ear is when there is thick fluid behind the eardrum that doesn’t clear away - but there is no infection present.
See the page on glue ear to learn more.
Are there other types of ear infections?
Outer ear infections
Tamariki can also get ear pain caused by infection of the skin around the outer part of the ear.
Outer ear infections are usually caused by water going into the ear, often after lots of swimming. This kind of infection happens more easily if they have skin conditions like eczema, which causes dry or broken skin in the ear canal.
See the page on outer ear infections to learn more.
Outer Ear Infections In Children
How middle ear infections happen
Middle ear infections often happen either during or just after a cold, when there are bacteria or viruses present in the back of the nose. They can travel up the eustachian tube from the back of the nose to the space behind the eardrum (middle ear). This happens more easily in young tamariki when the eustachian tube is short.
The infection causes swelling and can block the eustachian tube, which means air cannot reach the middle ear. Fluid and pus collect in the middle ear. The eardrum becomes red and inflamed and can bulge outwards. The inflammation and stretching of the eardrum is what causes ear pain. While there is fluid behind the eardrum, your child’s hearing can be reduced. Some tamariki with an ear infection can also have a fever.
The pressure that builds in the middle ear can sometimes cause the eardrum to burst.
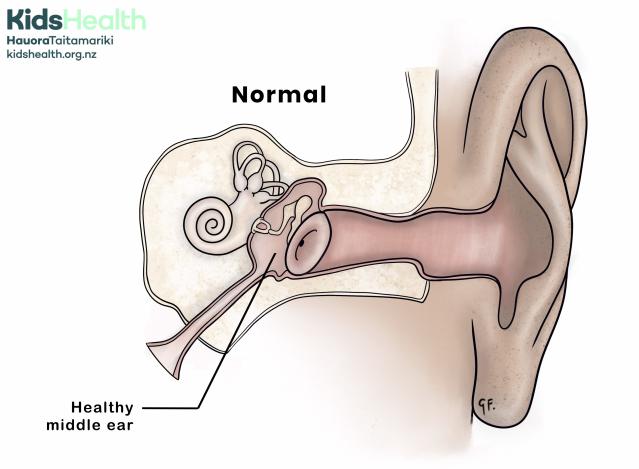
An illustration showing a normal, healthy middle ear with no fluid or inflammation.
Source: KidsHealth
transcribeTranscript
The illustration shows a cross-section of the ear, including the ear canal, eardrum, middle ear, and inner ear.
- The middle ear space behind the eardrum is clear and labelled Healthy middle ear.
- The cochlea and Eustachian tube are visible.
- The word Normal appears above the image
The KidsHealth logo with the website kidshealth.org.nz is in the top left corner.
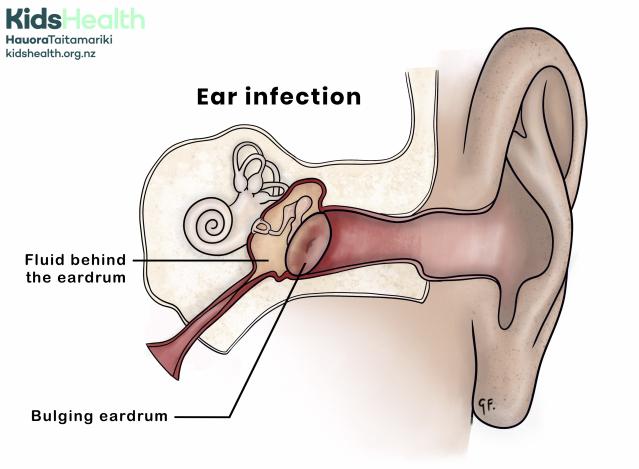
An illustration showing inflammation and fluid behind the eardrum during an ear infection.
Source: KidsHealth
transcribeTranscript
The illustration shows a cross-section of the outer, middle, and inner ear.
- The middle ear area is red and filled with fluid behind the eardrum, which is labelled and shown as swollen.
- The eardrum appears bulging due to pressure from the trapped fluid.
- The cochlea and Eustachian tube are visible.
At the top left is the KidsHealth logo with the website: kidshealth.org.nz.
Who gets ear infections
Ear infections are most common in pēpi (babies) and young tamariki. They are more likely to develop ear infections than older tamariki and adults. This is because their eustachian tubes (connecting the middle ear to the back of the nose) don't function as well as in older tamariki and adults - the tubes are smaller, shorter and flatter (more horizontal).
As tamariki grow older, their eustachian tubes work better and they also tend to get fewer colds. As a result, they usually outgrow having ear infections at around 7 or 8 years of age. But, some tamariki may have problems beyond this age.
Things that put children at risk of getting ear infections
We know some important risk factors, but not all the reasons why some tamariki develop more ear infections than others. The most important risk factors include:
- a family history of ear infections
- living with someone who smokes
- going to early childcare - pēpi and tamariki are exposed to more colds and viruses
- having an older brother or sister in childcare or early primary school
- the season - ear infections are more common during the autumn and winter months
- having significant nasal allergies (allergic rhinitis or 'hayfever')
Can you catch middle ear infections?
Ear infections cannot be passed on from one person to another, but the cold or other infection which caused them can.
Signs and symptoms of an ear infection
The pain from an ear infection usually comes on quickly and doesn't last long. It usually wears off within 24 hours.
Symptoms in older children
Symptoms of an ear infection in older tamariki can include:
- significant ear pain
- fever
- feeling unwell
- complaints of reduced hearing in the affected ear
- problems with balance
Symptoms in babies and younger children
In pēpi and younger tamariki, sometimes the only sign of an ear infection is a fever.
Younger tamariki may also:
- cry a lot and become generally irritable
- be hard to settle and have very disturbed sleep, getting more upset when they lie down
- become 'clingy' and 'grizzly'
- not drink or eat as much as usual
Burst ear drum
Sometimes pus will burst through the eardrum. The pus can look like snot coming out of the ear. When the eardrum bursts, tamariki often feel better as the pressure causing the pain is suddenly released. The burst eardrum usually heals without treatment or future problems.
See a health professional if you think your child has a burst eardrum. The health professional may give your child antibiotic ear drops.
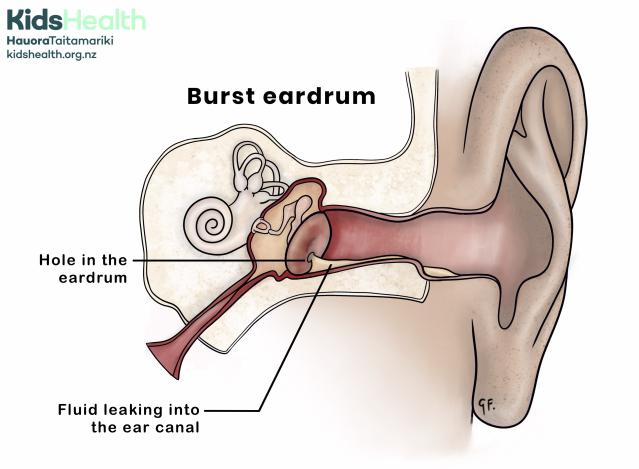
An illustration showing a burst eardrum, where fluid leaks from the middle ear through a hole in the eardrum.
Source: KidsHealth
transcribeTranscript
The illustration shows a cross-section of the ear, including the outer, middle, and inner ear.
- The eardrum has a hole, labelled hole in the eardrum.
- Fluid is shown leaking into the ear canal from the middle ear.
- The middle ear remains red and inflamed.
At the top left is the KidsHealth logo with the website: kidshealth.org.nz.
When to get medical help for your child
If you think your child may have an ear infection, see a health professional. They will talk to you about your child’s symptoms and look into their ears with an otoscope. An otoscope is a small powerful light with a magnifying lens.
A video showing a health professional looking inside a young boy's ear canal with an otoscope.
Source: KidsHealth
Holding your child while the health professional looks in their ears
Most pēpi and tamariki do not like having their ears examined. To make it easier, your health professional will probably encourage you to:
- hold your child sitting sideways on your lap
- wrap one of your arms gently over their arm
- gently hold their head against your chest with your other hand

Photo showing how to comfort and hold your child during an ear exam.
Source: KidsHealth
Managing an ear infection
Pain relief
Regular pain relief is important to help your child feel more comfortable. Paracetamol and/or ibuprofen can help reduce pain and lower fever, which can make your child feel better. You must follow the dosage instructions on the bottle. It is dangerous to give more than the recommended dose.
Antibiotics are often not needed
Ear infections do not usually need treatment with antibiotics, particularly if your child is over 2 years of age. After one week, at least 3 out of 4 tamariki will be better, whether they take antibiotics or not.
The decision about whether or not to use antibiotics may depend on some of the following:
- whether your child has a high fever or severe pain
- how old your child is - your health professional is more likely to give antibiotics if your child is under 2 years old
- if your child still has pain or discomfort after 48 hours of pain relief
- how often your child has had middle ear infections before
- whether your child has ever had complications from ear infections before, like a burst eardrum
- whether your child has any other medical conditions
- your views on how to best manage your child's ear problems
Caring for your child with an ear infection at home
Things you can do at home when your child has an ear infection include:
- giving your child regular pain relief, as recommended by your health professional
- giving your child lots of comfort and cuddles
- letting your child rest
- keeping your child home from child care or school while they are unwell or have a fever
There is no evidence that decongestant medicines (including nose sprays) and antihistamines are of any benefit in the treatment of acute ear infections. Don't use them as they can have unwanted side effects.
How long an ear infection can last
The pain from an ear infection comes on quickly, but usually doesn't last long. It usually improves within 24 to 48 hours.
After an ear infection, it is normal to have some fluid behind the eardrum (effusion). This can take a few weeks to drain away (down the eustachian tube). It may cause your child to have an ongoing feeling of discomfort or blockage in their ears. It is more a dull, abnormal feeling than a nasty, sharp pain. The fluid also causes a short-term decrease in hearing in that ear, which goes back to normal as the fluid clears away. They may hear some crackling or popping noises, which is a good sign that the fluid is clearing.
When to go back to a health professional for an ear infection
Once an ear infection is diagnosed, your child should start to improve within 24 to 48 hours. Go back to a health professional if:
- an earache is not settling after 2 days
- fluid starts coming out of your child's ear
- your child seems more unwell
There are some very rare complications of ear infections. Go back to a health professional urgently if your child:
- has any swelling, redness or tenderness in or around the ear (this could be mastoiditis)
- is feeding poorly
- is floppy, sleepy or drowsy
- is becoming less responsive
- is not interested in surroundings (lethargic)
- complains of a stiff neck or light hurting their eyes (this could be meningitis)
Frequent ear infections
If your child gets frequent ear infections, they may need to see an ENT (ear, nose and throat) specialist to consider grommets.
Possible long-term complications from ear infections
Most tamariki outgrow ear infections and will have normal, undamaged ears and normal hearing.
The fluid that collects behind the eardrum (called an effusion) can last for weeks to months after the pain of an ear infection is over. The fluid clears up within 12 weeks for 80% of tamariki.
Hearing loss
Hearing loss is the main complication of ear infections. Make sure your child has the B4 School Check and has their hearing tested.
A hole in the eardrum that doesn't heal
If your child has had a hole in the eardrum (eardrum perforation) after an infection, it will usually heal on its own. If perforation happens more than once, or if the infection causes a larger hole, sometimes it doesn’t heal. Tamariki can sometimes need an operation to repair the hole, but usually this isn’t done until after the age of 8.
A hole in the eardrum can sometimes cause problems with frequent leaking from the ear. Your child may need earplugs or other measures to try to keep their ear healthy until they are old enough to have the hole repaired.
Preventing ear infections
It is not easy to prevent ear infections, but the following may help reduce the risk:
- making sure your child's environment is smoke-free
- breastfeeding your baby for ideally at least 6 months is thought to be protective against the early development of ear infections - this may be because breastfeeding boosts the immune system
- keeping your child's room warm and dry
- making sure your child has all their vaccinations on time
Acknowledgements
Illustrations by Dr Greta File. Property of KidsHealth.
