Key points about meningococcal disease
- meningococcal disease is a bacterial infection - it causes severe illness and can cause death
- pēpi and tamariki with meningococcal disease can get sick very quickly
- meningococcal disease can be difficult to diagnose in its early stages
- take your child to a health professional urgently if they appear very ill, especially if there is a rash
- take your child back to your health professional urgently if they get worse
- know about the early symptoms of meningococcal disease and teach teenagers about these too
- know where to seek help after hours and how to get there
- early treatment can save lives
Find out about protecting your child against meningococcal B disease.
Meningococcal B Disease Vaccination
What is meningococcal disease?
Meningococcal disease is an infection caused by a bacteria. It can lead to 2 very serious illnesses:
- meningitis (an infection of membranes that cover the brain)
- septicaemia (a serious infection in the blood)
Some tamariki will have both meningitis and septicaemia, others will have one or the other.
There are several different types of meningococcal bacteria including A, B, C, Y and W.
How common is meningococcal disease?
Between 1 January to 31 December 2023 there were 59 cases of meningococcal disease in Aotearoa New Zealand. Of these cases, 15 were in tamariki aged under 5 years old.
It's more common in winter and spring. The highest rates of meningococcal disease occur in tamariki aged under 5 years and young people aged 15 to 19 years. But, people of any age can be affected.
How meningococcal disease spreads
Meningococcal disease can easily spread from person to person.
The bacteria can spread through close contact such as:
- living in the same household
- coughing and sneezing
- kissing, sharing food, drinks and utensils
Why only some people exposed to meningococcal bacteria get sick
Some people will carry meningococcal bacteria in their nose and throat without getting sick.
Scientists and health professionals don't yet know why some people who come into contact with meningococcal bacteria get sick and others don't.
Who is most at risk of catching meningococcal disease
Meningococcal disease can affect anyone, but some people have an increased risk:
- tamariki and rangatahi (young people) under 20 years (particularly pēpi under one and tamariki under 5)
- tamariki and rangatahi who live in shared accommodation (like hostels and tertiary halls of residence)
Signs and symptoms of meningococcal disease
Symptoms may appear in any order and some may not appear at all. In the early stages of meningococcal disease, symptoms may seem similar to those of the flu or any other viral infection. The disease can develop very quickly and is difficult to diagnose.
It's important to be aware of the symptoms so you can get medical help straightaway - whether it's day or night.
Meningococcal disease can be treated with antibiotics but early treatment is very important.
Know about the early symptoms of meningococcal disease and take action if you are concerned.
Symptoms in a baby or child who has meningococcal disease
A baby or child with meningococcal disease may:
- have a fever (may also have cool hands and feet, or shivering)
- be crying or unsettled
- refuse drinks or feeds
- vomit
- be sleepy or floppy or harder to wake
- dislike bright lights
- have a stiff neck
- have a bulging fontanelle (the soft area on the top of a baby's head)
- have red or purple spots or bruises on the skin
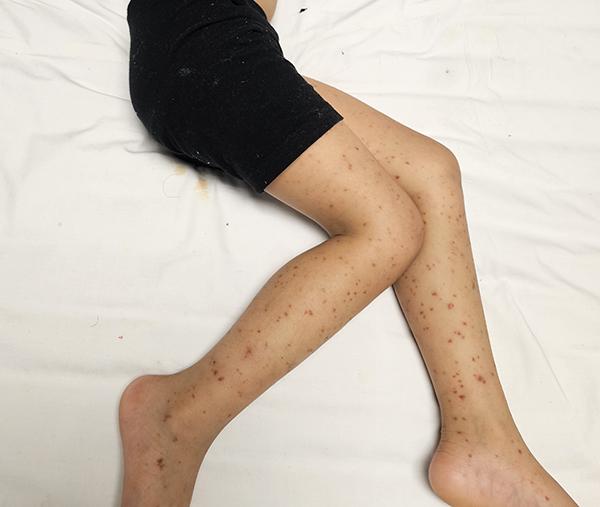
Photo of a meningococcal rash on a child's legs (be aware only 1 in 3 tamariki with meningococcal disease have a rash).
Source: KidsHealth
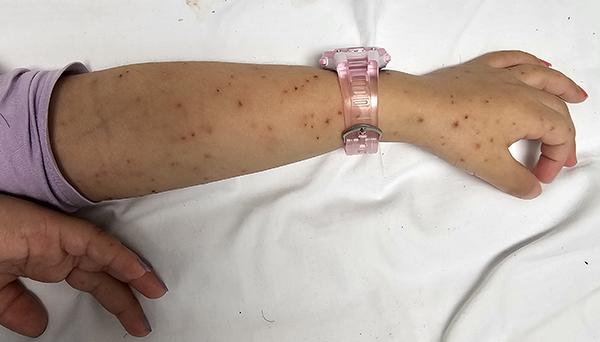
Photo of a meningococcal rash on a child's arm (be aware only 1 in 3 tamariki with meningococcal disease have a rash).
Source: KidsHealth
Symptoms in an older child or adult who has meningococcal disease
An older child or adult with meningococcal disease may:
- have a fever or a headache
- have a stiff neck
- have joint pain and aching muscles
- vomit
- be sleepy, confused, delirious or unconscious
- dislike bright lights
- have red or purple spots or bruises on the skin (see the photos above but be aware only 1 in 3 tamariki and adults with meningococcal disease have a rash)
When to get medical help for your child
If your child has one or more of the symptoms of meningococcal disease:
- act immediately
- ring your doctor's clinic, after hours medical centre or Healthline (0800 611 116) right away - whether it’s day or night
- if it is an emergency, call 111 within New Zealand and ask for an ambulance (use the appropriate emergency number in other countries)
- say what the symptoms are
- insist on immediate action - don't be put off - a life may be at risk
- watch your child, even if they have already been checked by a health professional - ask your health professional what to look out for
- go straight back to a health professional if your child gets worse
- do not leave your child alone
Healthline is available 24 hours a day, 7 days a week on 0800 611 116. Call Healthline if you need advice about a child of any age who is unwell, hurt, or has any symptoms of sickness. It's free to callers throughout New Zealand, including from a mobile phone.
Treating meningococcal disease
Early treatment of meningococcal disease with antibiotics is very important. It can save lives and reduce the effects of the disease.
Preventing meningococcal disease in close contacts
Once the healthcare team diagnoses meningococcal disease in someone, they give antibiotics to that person's close contacts. This treatment clears the organism from their throat and prevents the spread of meningococcal disease from person to person.
Vaccination for meningococcal disease
There are several different types of meningococcal bacteria including A, B, C, Y and W. In Aotearoa New Zealand, most meningococcal disease is caused by group B bacteria.
Vaccination against meningococcal disease is important. Meningococcal disease can develop quickly and be life-threatening. The meningococcal vaccines protect against the bacteria that cause meningococcal disease.
There are 2 types of meningococcal vaccine in Aotearoa New Zealand:
- The MenB vaccine - protects against meningococcal B
- The MenACWY vaccine - protects against meningococcal A, C, W and Y
Children under 5 years old
The MenB vaccine has been part of the National Immunisation Schedule for pēpi since March 2023. Pēpi usually have the MenB vaccine at 3 months, 5 months and 12 months old.
Your baby can have the MenB vaccine as part of their regular scheduled vaccinations.
There is also an option for your baby to have the MenB vaccine slightly earlier at 2 months, 4 months and 12 months old. This will involve extra appointments. You can talk to your health professional about this during your baby’s 6-week check appointment.
Children and young people aged 13 to 25 years old
MenACWY and MenB vaccines are free for tamariki and rangatahi aged 13 to 25 years in their first year of close-living situations. They can get their vaccine up to 3 months before entering a close-living situation. Close-living situations include boarding schools and hostels, military barracks and tertiary halls of residence. It doesn’t include flatting.
Talk to your health professional to see if this is recommended for your child or young person.
Children with certain medical conditions
Extra meningococcal vaccines and doses may be free for tamariki with certain medical conditions. This is if their condition puts them at higher risk of meningococcal disease. This may include both the MenB and MenACWY vaccine.
Your health professional will talk to you about this if it is recommended for your child.
Close contacts of a person with meningococcal disease
Extra meningococcal vaccines and doses may be free for close contacts of someone with meningococcal disease. This includes both the MenB and MenACWY vaccine.
Talk to your health professional to see if this is recommended for you and your whānau.
Possible complications of meningococcal disease
For every 100 people who get the disease, 5 to 10 will die. Another 20 are likely to be left with some degree of serious disability, such as brain damage, deafness, loss of limbs or damaged skin. Some are also left with learning or behavioural difficulties.
More information and resources

Visit the HealthEd website for a resource on meningococcal disease symptoms and what to do if someone has them. You can read the resource in your preferred language.
English
Te reo Māori
Te Reo Māori Kūki ‘Āirani (Cook Islands Māori)
Te Gagana Tokelau (Tokelau)
Vagahau Niue (Niuean)
Vosa Vakaviti (Fijian)
Te taetae ni Kiribati (Kiribati)
Te Gana Tuvalu (Tuvalu)

See the HealthEd website for the 'Don't wait, take action' poster. It includes the symptoms of meningococcal disease in babies and children. The poster is available in English, te reo Māori, Samoan and Tongan.
English
Te reo Māori
Lea Faka-Tonga (Tongan)
Gagana Samoa (Samoan)

Check the Meningitis Foundation website for information and resources, including personal stories and podcasts.

Ripu Bhatia was a 21-year-old university student living in Sydney when he had his arms and legs amputated after getting meningococcal disease. You can read Ripu's story at the Stuff website.
Mark and Lisa's experience of meningococcal C disease in their daughter Letitia
You can watch a video of a family's experience of meningococcal C disease. In the 5 hours between waking at 3am with a headache and 8am when her family had gathered at Palmerston North Hospital, 18-year-old Letitia (Tesh) Gallagher's body had battled meningococcal C disease.
Mark and Lisa Gallagher share the story of their daughter Letitia (Tesh) and her battle with meningococcal C disease.
Source: Ministry of Health
transcribeTranscript
Transcript
[Mark] It started on a Sunday night. Our daughter came for dinner, as she usually does on a Sunday night, with her boyfriend but she wasn't very well, she had a bit of a temperature so she didn't eat anything.
She then went to bed that night with a bit of a headache, so she took some Panadol.
She woke up at about 3 in the morning with a very very painful head. Thankfully her boyfriend was there and he rang an ambulance straight away and they shot her straight through to Palmerston A and E.
We both got there and we were pretty shocked as to what we saw. It was a pretty horrific thing to see.
We were told that ICU would be closed for a couple of hours while the doctors do their rounds.
We were asked to just go away and have a coffee and freshen up and then come back in an hour or so. We only got down as far as the car park. The boyfriend stayed in the waiting room, he text us and said "Look, you better come back, there's been a development".
We came back and they took us into another room and said "Look, she's pretty bad, there's nothing they can do for her. She's dying".
And that was at 8:30. So in the space of 5 hours, she'd gone from a headache and fever to nothing they can do. The only real symptoms was the headaches, the temperature, the vomiting and that was pretty much it.
I mean OK, they have a lot of symptoms with meningitis, not all of them show straight away, that's the thing we found.
So you're better to be safe than sorry.
We didn't know, we had no idea. It's not until now that we realise that, OK Men [Meningococcal] C, you can actually get a separate vaccine to that, Men B one to the Men A one, so there's lots of different strands of it.
So unfortunately, yeah she wasn't immunised against Men C.
Yeah, we've been very active.
We've been down to Parliament for the launch of a new immunisation campaign and just the awareness of it all and getting the awareness of out there to, you know, make people immunised and tell them about it and get them to say look, ya know, start talking about it. And that's what it's all about, it's a matter of getting your people to be aware of it, get the immunisation out there and get their kids vaccinated.
So yeah we've done a bit, we're doing our best.
[Lisa] And we still will.
[Mark] And we will, we definitely will. Yeah we've got a lot more to do yet.
[Lisa] Keep going.
[Mark] Our daughter would be kicking our butts if we didn't!
Acknowledgements
This content has been produced by the Paediatric Society of New Zealand in collaboration with the Immunisation Team, Ministry of Health.

