Key points about mitochondrial disease
- we all have mitochondria - they are found in every cell in our body
- mitochondria are the tiny parts of our cells that are responsible for making energy and are known as the 'powerhouse' or battery of the cell
- mitochondrial disease or 'mito' is caused when our mitochondria are faulty and therefore unable to produce enough energy
Receiving a diagnosis of mitochondrial disease
A diagnosis of mitochondrial disease can, understandably, be devastating. There will be many questions and emotions. This page aims to provide information and support for New Zealanders affected by mito, along with their whānau and friends.
What are mitochondria?
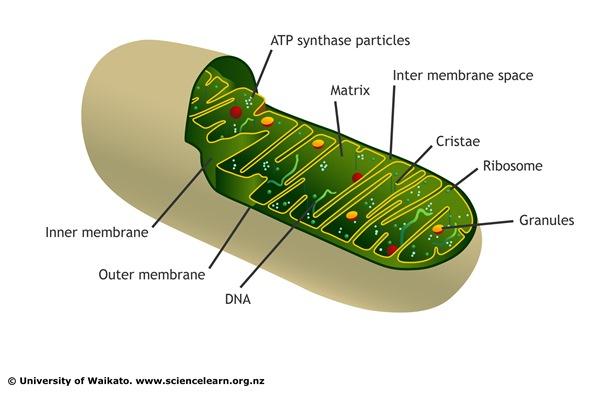
There are mitochondria in every cell in our body. They are the tiny parts of our cells that are responsible for making energy - the 'powerhouse' or battery of the cell. Through a series of complex chemical reactions, they turn glucose and oxygen into an energy chemical called ATP. This chemical process is called oxidative phosphorylation. They also produce energy from fat (fatty acid oxidation). When the mitochondria don't work properly, the cell has a power failure and the affected organ begins to shut down. This power failure is called mitochondrial disease.
What is mitochondrial disease?
Mitochondrial disease or Mito is caused when our mitochondria are not working properly. Mitochondrial dysfunction can result in damaged cells and organ failure. The damage can be triggered when the body is under significant stress, such as during illness. Mito can be a degenerative disease that usually targets the parts of our body that require the most energy such as the brain, heart, kidneys and muscles. However, any organ system at any age can be affected. At present, there is no cure for mitochondrial disease.
Signs and symptoms of mitochondrial disease
The severity of Mito symptoms differs from person to person, even within the same family. Everyone's journey is different. Many people will have multi-organ disease. In babies, the brain is often involved. Some symptoms might be:
- normal development followed by loss of skills
- poor growth, difficulty tolerating feeding
- stroke-like events affecting specific parts of the brain
- seizures
- poor coordination, tremor or delay in reaching motor developmental milestones
- muscle weakness (hypotonia or myopathy)
- learning disability in children or early dementia in adults
- reduced eye movement (ophthalmoplegia), loss of vision or drooping eyelids (ptosis)
- neurological deafness
- thickening of the heart or abnormal heart rhythms
- liver or kidney disease or failure
Adults may present with early-onset diabetes and multiple miscarriages.
Why mitochondrial disease happens
All of the proteins in our body are made from DNA - our genetic material that makes us human. We have 2 types of DNA:
- Our nuclear DNA (nDNA) which we inherit from both parents. There are over 20,000 genes in our nDNA. Over 1,000 are involved in helping the mitochondria function.
- Mitochondrial DNA (mtDNA) which is inherited from our mother as only the egg contains mtDNA. This is a ring of DNA found in every mitochondria. It contains 37 genes.
Mitochondrial disease can be caused by one of the following:
- a fault (mutation) in the nDNA that is inherited from both parents (autosomal recessive inheritance)
- a mutation in the mtDNA that can be maternally inherited (mtDNA inheritance)
- a mutation in the mtDNA or nDNA that seemingly occurs for the first time in the affected individual (de novo)
- a mutation in nDNA passed down from one affected parent (autosomal dominant or X-linked)
Diagnosing mitochondrial disease
There is no easy test to diagnose mitochondrial disease. Reaching a diagnosis often requires putting pieces of a jigsaw puzzle together. Many symptoms of Mito are similar to those of other illnesses. Symptoms may be erratic, at first subtle, further complicating the journey to diagnosis.
Clinical and radiological features, blood, urine and other biochemical tests can strongly suggest mitochondrial disease. DNA testing, and to a lesser extent, muscle biopsies are usually required to confirm Mito. Sometimes a specific genetic diagnosis cannot be achieved so a diagnosis of 'suspected mitochondrial disease' is made based on all of the clinical and biochemical features. Our understanding of the genetic basis of Mito is growing all the time. A specific genetic diagnosis can help whānau understand the condition better, know what to expect for the future and help them make decisions about future pregnancies.
Managing mitochondrial disease
Living with mitochondrial disease can be very challenging and demanding physically, psychologically, and emotionally for the person affected, their friends and whānau. There are currently no medically proven treatments for Mito. However, there are some clinical trials, and there is some promising research underway for some diseases. Some people can respond very well to certain vitamins or specific therapies depending on the genetic diagnosis.
For most people, 'treatment' is about supportive care, focussed around accurate and timely diagnosis, symptom management, maintaining good nutrition, avoiding illness where possible and avoiding certain medications that can damage the mitochondria. Some doctors recommend a 'mitochondrial vitamin cocktail' to help support the mitochondria. However, there is no evidence that this is beneficial for most mitochondrial diseases.
Who helps manage mitochondrial disease in New Zealand
Patients with mitochondrial disease can sometimes require a team of people to help manage their symptoms and issues. This team can include the family, neurologist, ophthalmologist, community nurses, GPs, psychologists, social workers, physiotherapists, speech-language therapists, dietitian or palliative care specialists.
The Adult and Paediatric National Metabolic Service, based at Starship Children’s Hospital, look after adults and children around the country with mitochondrial disease. The metabolic specialists (children and adults) are Dr Callum Wilson, Dr Bryony Ryder and Dr Emma Glamuzina. They and their team can help coordinate with local specialists and other team members. They work within an international network of specialists and researchers in mitochondrial disease.
Don't give up hope - don't let the power go out!
More information and support

Parent to parent is a nationwide not-for-profit organisation formed in 1983 by parents and professionals to support the families of people with any type of disability or health impairment. Check their website to learn more about their services and how they can help.

UMDF supports research and education for the diagnosis, treatment and cure of mitochondrial disorders and to provide support to affected individuals and families. Their website has information for health professionals as well as individuals and their families.

The Lily Foundation is the UK's leading charity dedicated to fighting mitochondrial disease. Their mission is to support people whose lives are affected by the condition, raise awareness and fund research into its prevention, diagnosis and treatment.
Acknowledgements
This page has been written by parents of children with mitochondrial disease and supported by the NZ National Metabolic service and has been reviewed by metabolic specialists. It is also based on the pamphlet Mitochondrial disease (PDF, 832KB).
