Key points about supraventricular tachycardia (SVT)
- an abnormally fast heart rhythm is called tachycardia
- tachycardias can arise from the upper or lower chambers of the heart
- tachycardias that involve the upper chambers are called supraventricular tachycardia
- supraventricular tachycardias are usually not dangerous
- they are not due to a 'heart attack' and in tamariki (children) with an otherwise healthy heart, do not cause sudden death
What is supraventricular tachycardia (SVT)?
An abnormally fast heart rhythm (tachycardia) can arise from the upper or lower chambers of the heart, or can be a 'circuit' made up of the upper and lower chambers. Doctors can see the heart's electrical activity by using an electrocardiograph (ECG).
Tachycardias that originate from the lower chambers (the ventricles) are called ventricular tachycardia. Those that involve the upper chambers (the atria) are termed supraventricular tachycardia (SVT).
Supraventricular tachycardias are usually not dangerous. They are not due to a 'heart attack' and in tamariki with an otherwise healthy heart, do not cause sudden death. However, if they occur very often or for long periods of time (hours to days), then they can cause difficulty with the pumping action of the heart. This can be dangerous if untreated.
The SA node is the normal pacemaker of the heart. The AV node sits between the upper and lower chambers of the heart. Electrical activity moves from the SA node to the AV node and then down through the heart.
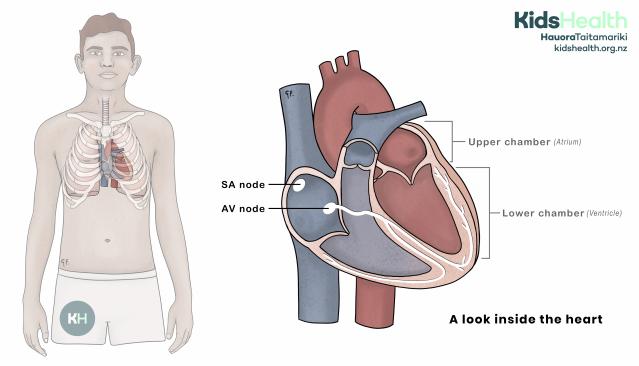
This illustration shows the heart’s location in the chest and a close-up view of its chambers and the SA and AV node. Electrical activity moves from the SA node to the AV node and down through the fibres illustrated in white.
Source: KidsHealth
transcribeTranscript
On the left, the illustration shows a teenage male. The ribcage is visible, with the heart shown inside the chest between the lungs.
On the right, there is an enlarged cross-section of the heart. The heart has two upper chambers (atria) and two lower chambers (ventricles). Two small white circles inside the right atrium are labelled SA node and AV node. Thin white lines run through the heart muscle, showing the heart’s electrical conduction pathways.
The text beneath reads: ‘A look inside the heart.’
At the top right is the KidsHealth logo with the website: kidshealth.org.nz
Normal conduction
Normal conduction of electrical signals through the heart starts with the SA node. Then it travels to the AV node and down through the ventricles.
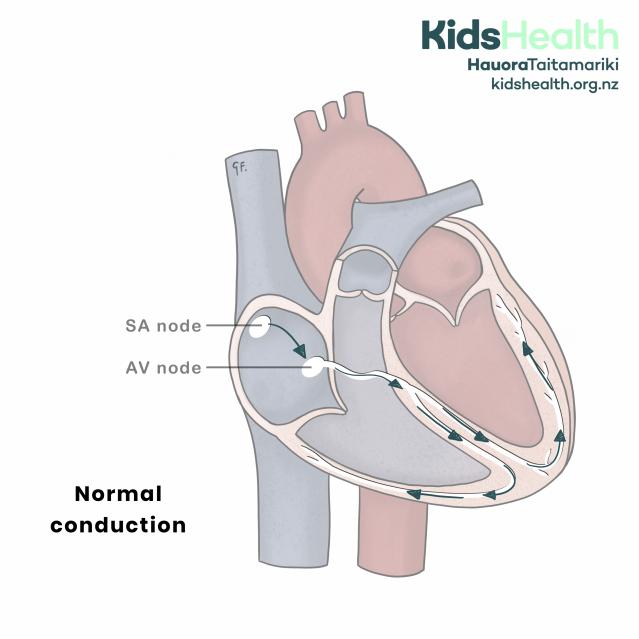
Normal conduction of electrical signals through the heart.
Source: KidsHealth
transcribeTranscript
The illustration shows a simplified cross-section of the heart. The right atrium contains the SA node (sinoatrial node) at the top and the AV node (atrioventricular node) lower down. Curved arrows show the pathway of electrical activity through the heart:
- Starting at the SA node in the right atrium
- Moving to the AV node
- Travelling down into the ventricles and spreading through both lower chambers via the branches (shown in white).
The text at the lower left reads: ‘Normal conduction’.
At the top right is the KidsHealth logo with the website: kidshealth.org.nz
Types of SVT
Atrial tachycardia
An area of the upper chambers takes over the pacemaker activity of the heart. This is relatively uncommon in tamariki.
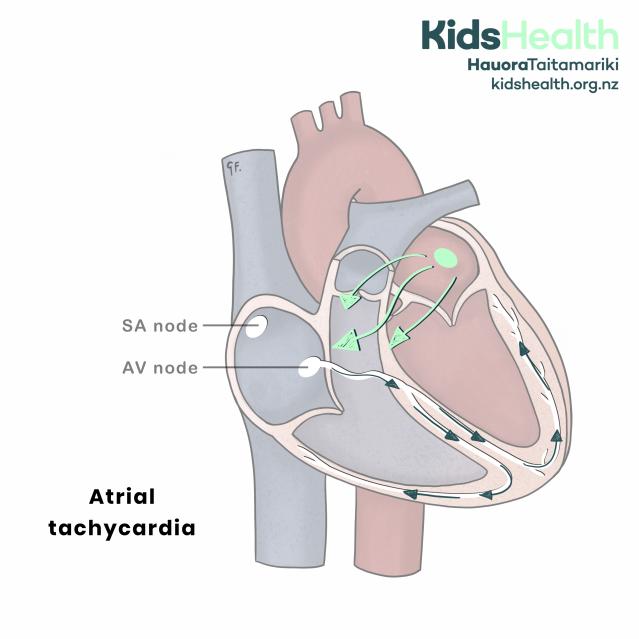
Atrial tachycardia.
Source: KidsHealth
transcribeTranscript
The illustration shows a simplified cross-section of the heart. The right atrium contains the SA node at the top and the AV node lower down. In this diagram, a green dot and arrows in the upper right atrium show an abnormal starting point for the electrical impulses, instead of starting at the SA node.
Green arrows trace the abnormal signals from the atrium to the AV node, and dark blue arrows continue from the AV node into the ventricles, spreading through both lower chambers.
The text at the lower left reads: ‘Atrial tachycardia’.
At the top right is the KidsHealth logo with the website: kidshealth.org.nz
Atrial Flutter
A large area of the upper chamber forms an electrical circuit. Tamariki who have had previous heart surgery involving the upper chambers usually display this rhythm. Some tamariki with atrial flutter are at risk of developing clots because the blood flow in these chambers is slow and disorganised.
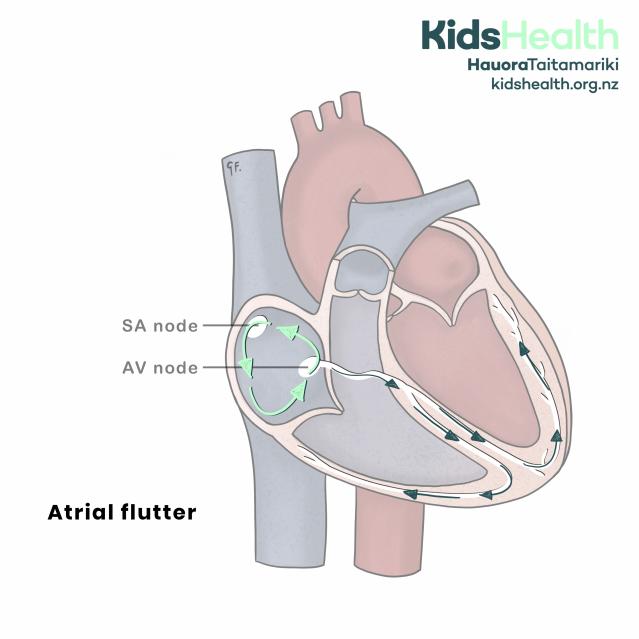
Atrial Flutter.
Source: KidsHealth
transcribeTranscript
The illustration shows a simplified cross-section of the heart. The right atrium contains the SA node at the top and the AV node lower down. In this diagram, green arrows show a continuous loop of abnormal electrical signals circling inside the right atrium.
The text at the lower left reads: ‘Atrial flutter’.
At the top right is the KidsHealth logo with the website: kidshealth.org.nz
Atrio-ventricular re-entrant tachycardia (AVRT)
An extra electrical connection (called an 'accessory pathway') exists between the upper and lower chambers. The wave of electricity that normally passes from the top to the bottom of the heart can now pass back up through the abnormal pathway, forming a re-entry circuit. This is the most common form of SVT in tamariki under 8 years of age. The majority of infants with atrio-ventricular re-entrant tachycardia 'outgrow' the tachycardia during their first year but it may come back in later childhood.
Specific diagnoses falling into this category include Wolff-Parkinson-White Syndrome (WPW) and permanent junctional reciprocating tachycardia (PJRT). In older tamariki, WPW is can in rare cases be life-threatening. Your child's doctor may recommend special tests and curative treatment known as an ablation. This is a type of 'keyhole' procedure where a surgeon will access the heart via the veins at the top of the leg.
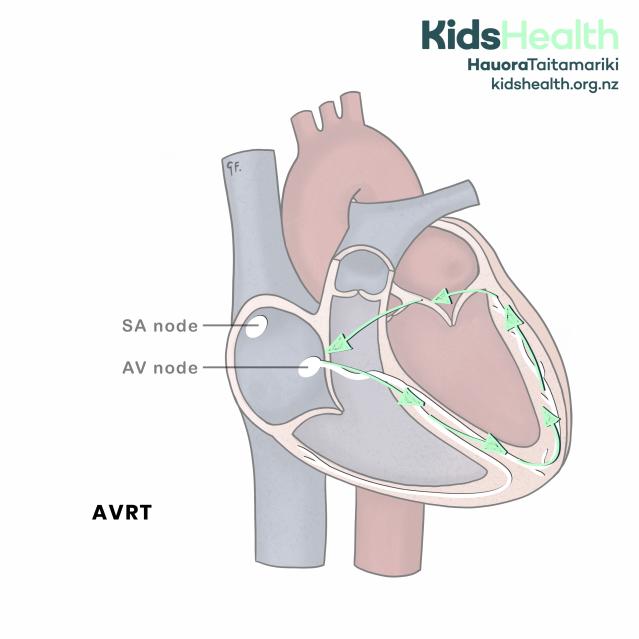
Atrio-ventricular re-entrant tachycardia (AVRT).
Source: KidsHealth
transcribeTranscript
The illustration shows a simplified cross-section of the heart. The right atrium contains the SA node at the top and the AV node lower down. Green arrows trace the abnormal pathway:
- The signal travels from the SA node to the AV node,
- Down into the ventricles,
- Then back up into the atria through an extra pathway, creating a reentrant loop.
This looping pathway repeats rapidly, causing the heart to beat faster.
The text at the lower left reads: ‘AVRT’.
At the top right is the KidsHealth logo with the website: kidshealth.org.nz
Atrio-ventricular nodal re-entrant tachycardia (AVNRT)
The atrio-ventricular node is located between the upper and lower chambers of the heart. It is normally the only area that allows the electrical activity of the heart to pass from the upper chambers to the lower chambers. Sometimes this area can become the source for a tachycardia. This is the most common form of SVT in tamariki over 8 years of age.

Atrio-ventricular nodal re-entrant tachycardia (AVNRT).
Source: KidsHealth
transcribeTranscript
The illustration shows a simplified cross-section of the heart. The right atrium contains the SA node at the top and the AV node lower down. Green arrows form a small loop around the AV node, showing the abnormal pathway of the electrical signals.
From the loop, impulses travel into the ventricles, shown by dark blue arrows, and spread through both lower chambers. This looping pathway inside and around the AV node repeats rapidly, causing a fast heartbeat.
The text at the lower left reads: ‘AVNRT’.
At the top right is the KidsHealth logo with the website: kidshealth.org.nz
How to recognise if your child has SVT
Older tamariki and rangatahi (young people) often experience a fast heart rate as palpitations. They may feel their heart racing at unexpected times such as resting, doing homework, after exercise or eating dinner. Younger tamariki may have difficulty describing this sensation and may complain of chest pain. SVT may rarely cause tamariki or rangatahi to pass out (syncope).
Some newborns can be quite unwell if they have had SVT in the womb for a long time. In most infants, however, SVT is well tolerated as long as it is detected within a few hours of it starting.
You may notice the fast heart rate might be while cuddling your baby or during feedings. Some infants develop poor feeding, irritability, unnatural paleness and fast breathing if the SVT continues. If your baby has a fast heart rate very often or shows any of these signs, you should seek medical advice.
When to get urgent medical help for your child
During a bad attack, your child may become dizzy or less alert, pass out, feel cold, look pale or sweaty. Learning to take your child's pulse is an important skill that will help identify when the rhythm is too fast. If you feel a fast heart rate is causing your child to become seriously unwell, call an ambulance.
Always call an ambulance if your child passes out with an attack. If it is SVT, they should wake up quickly as soon as they lie down. Try 'vagal manoeuvres' (see 'How is an SVT attack stopped?' below). Keep your child lying down, or sitting until fully recovered.
Preventing SVT attacks
There are different medicines which your child can take by mouth (oral). These medicines prevent attacks when taken regularly. The choice of medication depends on the type of tachycardia. Common medicines include:
- Sotalol
- Flecainide
- Atenolol and Propranolol
- Amiodarone
Managing SVT attacks
Vagal manoeuvres
'Vagal manoeuvres' can stop an attack of SVT. These work by stimulating the vagus nerve in the chest causing the heart to slow. In an infant, you can try a cold (iced) flannel over their eyes for about 10 seconds. In hospital (only), doctors may immerse a baby's face under cold water for a few seconds.
Tamariki can put their thumb in their mouth and blow hard on it - until they go red in the face. A very cold drink, or standing on their head can work too.
Medicine
Doctors and nurses use intravenous medicines (medicines put directly into a vein) in hospital to stop an attack. The usual medicines are Adenosine and Amiodarone.
Electrical cardioversion
Electrical cardioversion is rarely needed. This involves using a controlled electrical shock to 'jolt' the heart back to a normal rhythm and happens under a brief general anaesthetic.
Can SVT be cured?
If the tachycardia lasts to school age, the SVT can be cured by physically disabling the part of the heart causing the problem. This is called radio-frequency ablation and involves a cardiac catheter study where the electrical pathways of the heart are clearly mapped and the problem area identified and disabled. It is usually done under a general anaesthetic, and the catheters (special wires) are passed to the heart from veins in the top of the leg.
Acknowledgements
Illustrations by Dr Greta File. Properly of KidsHealth.
This content has been written by health professionals in the Paediatric and Congenital Cardiac Service at Starship Children's Health, guided by Professor Jon Skinner and Diane Stephenson, Starship Children's Health.
