Key points about tongue tie
- tongue tie is a condition that involves a small piece of tissue (the frenulum) connecting the tongue to the bottom of the mouth
- tongue tie may cause a problem with breastfeeding for some pēpi
- some pēpi have difficulties latching on to the breast straight after birth even when they don't have a tongue tie
- it's very common to need a bit of extra support before you and your baby both become experts at feeding
- problems often go away as you both get better at breastfeeding
- most tongue ties do not cause any problems with speech or eating
- many pēpi born with a tongue tie don't have any problems breastfeeding and don't need any treatment
What is tongue tie?
Tongue tie is a condition that involves a small piece of tissue connecting the tongue to the bottom of the mouth. This is called the lingual (meaning tongue) frenulum, often just called the frenulum.
Everyone has a frenulum, and everyone's frenulum is a different length and thickness. Sometimes you can't see a person's frenulum. When a baby's frenulum is short or tight it can stop their tongue from moving properly. This is called a tongue tie (ankyloglossia).
Around 5% to 10% of pēpi are born with a tongue tie, but at least half of these pēpi can still breastfeed normally. That means around 2% to 5% of pēpi have a tongue tie that may cause a problem with breastfeeding or bottle feeding.
Why tongue tie can be a problem
Many pēpi born with a tongue tie don't have any problems breastfeeding and don't need any treatment. Some pēpi with tongue tie have difficulty latching on to the breast comfortably. Occasionally, pēpi with a severe tongue tie can also have problems bottle feeding.
Some pēpi have difficulties latching on to the breast straight after birth even when they don't have a tongue tie. Some pēpi with tongue tie and difficulty latching do not improve after the tongue tie is treated.
It takes time to learn how to breastfeed for both you and your baby. It’s very common to need a bit of extra support before you and your baby both become experts. Problems often go away as you both get better at breastfeeding.
Signs a tongue tie is causing problems
If your baby's tongue tie is making it difficult for your baby to breastfeed, you may notice some signs:
- breastfeeding is painful during the whole of the feed
- your nipples may become sore, blistered, cracked, bleeding or bruised
- a misshapen nipple after feeding
Your baby may:
- have difficulty latching on to the breast
- come on and off the breast during a feed
- make clicking or slurping noises while they are feeding
- take an extremely long time to feed
Getting a breastfeeding assessment
If you are worried about how your baby is feeding, ask to have a breastfeeding assessment.
Talk to your midwife or LMC
Your midwife or lead maternity carer (LMC) can refer you to a lactation consultant for an assessment. A lactation consultant is a professionally trained breastfeeding specialist.
The referral process will vary across the country, and your midwife/LMC will know who to refer you to in your area.
Talk with a PlunketLine nurse
You can also talk to a PlunketLine nurse on 0800 933 922. Calls are free and PlunketLine is available 24/7. They'll do an assessment and can book you an online appointment with one of Plunket's lactation consultants.
These breastfeeding consultations are free and available for all breastfeeding women - even if Plunket isn’t your WellChild provider.

Check out SmartStart to find breastfeeding support services in your area.
What happens during a breastfeeding assessment
During the assessment, a lactation consultant will talk to you about your baby's feeding. They will watch your baby breastfeeding and adjust your breastfeeding technique if necessary. They will also look at how your baby's tongue is moving and how their frenulum is attached.
The lactation consultant will use a simple scoring tool to assess the tongue-tie.
You and your baby can have a breastfeeding assessment as early as 2 days after they are born if your baby has severe feeding problems. Talk to your midwife if you are worried.
Treatments for tongue tie in babies
For many pēpi with tongue tie, it is best to wait and see how feeding goes. It's important that you receive support for your breastfeeding.
If breastfeeding is still difficult and the lactation consultant thinks your baby's tongue-tie is causing problems, they may suggest your baby has a tongue-tie release. This is sometimes called a tongue-tie snip, a division of the frenulum, or a frenotomy. This may make it easier to breastfeed.
If my baby needs treatment for tongue tie, who will do it?
Your lactation consultant or midwife can refer your baby to a health professional trained in tongue tie release. This can happen through the public health system, or you can pay to have it done privately. Talk to your lactation consultant or LMC about what will suit you best.
The following health professionals can do a tongue tie release:
- some registered midwives (they may also be a lactation consultant)
- some general practitioners (GP)
- some paediatricians
- some dental surgeons
- some ear, nose and throat (ENT) surgeons
Preparation for a tongue tie release
Your baby must have had vitamin K before having a tongue tie release. If they have not had Vitamin K, they cannot have the procedure.
Vitamin K For Newborn Babies To Prevent Serious Bleeding
Your baby will be wrapped securely (swaddled) and held carefully so they don't wriggle while having the procedure.
Your baby may be given a small amount of breast milk or sucrose (sugar) to help with pain.
What happens during a tongue tie release
A tongue tie release is a quick and simple procedure.
The health professional doing the tongue tie release will lift your baby's tongue and snip the frenulum with a pair of sterile scissors. There will be a small amount of bleeding. Your baby will experience some discomfort and may be upset about being wrapped and held firmly.
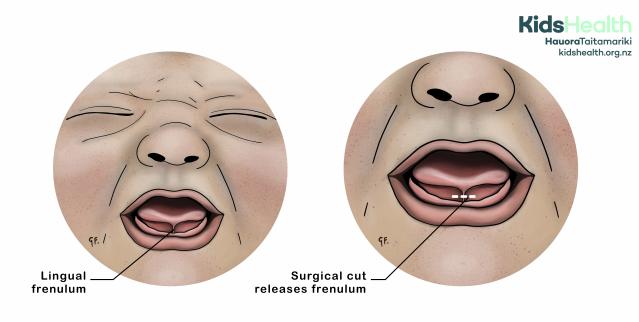
An illustration showing the lingual frenulum and the area where a surgical cut (frenotomy) would release it.
Source: KidsHealth
transcribeTranscript
The illustration shows two close-up views of a baby’s face and open mouth.
On the left, the baby’s mouth is open and the lingual frenulum — a small fold of tissue connecting the underside of the tongue to the floor of the mouth — is clearly visible. A label points to it with the text ‘Lingual frenulum’.
On the right, the baby’s mouth is open again. The frenulum is still visible, but now a dotted white line marks the area where a surgical cut would release the frenulum. The label reads ‘Surgical cut releases frenulum’.
At the top right is the KidsHealth logo with the website: kidshealth.org.nz.
Immediately after the release, your health professional will ask you to breastfeed your baby.
Most pēpi have a tongue tie release before they are 2 months old. If your baby is older, or has a more complicated tongue tie, they may need treatment under general anaesthetic by a surgeon.
What to expect after a tongue tie release
Some mothers notice a difference straight away after the tongue tie release, while others take a few days to see an improvement. Some mothers say it makes no difference.
You might see a small white/yellow patch under your baby's tongue a few days following the release. This can sometimes happen during the healing process and should disappear over a week or so. Your LMC can check this.
If the feeding difficulties continue, it may be that there are other problems affecting your baby's feeding, and your baby may need further assessment. Your midwife, GP, practice nurse, or Well Child Tamariki Ora nurse will follow up to see how you are doing. If you still have problems, they will see what can be done about them.
You should continue to get support with breastfeeding from your midwife or LMC. Talk to them if feeding is not improving or if you have any other worries.
Possible complications after a tongue tie release
Sometimes the wound under your baby's tongue may bleed after the tongue tie release once you get home.
You may notice slight oozing from the wound after breastfeeds and your baby may have slightly pinkish saliva. Or, if your baby spills after feeds, it may look pinkish.
If you notice any fresh blood in your baby's mouth, try feeding your baby.
The pressure of your nipple on your baby's tongue should help stop the bleeding in a few minutes.
If the bleeding is heavy or does not stop within 15 minutes following breastfeeding, or if you are unable to get your baby to take a feed, put direct pressure to the wound under your baby's tongue for 5 minutes. Use one finger and a clean piece of gauze or muslin. Do not apply pressure under your baby's chin as this can affect their breathing.
If bleeding continues after this time, continue to apply pressure and call an ambulance.
PlunketLine is available 24 hours a day, 7 days a week, on 0800 933 922 for advice and support for you, your baby and your whānau. Calls are free from cell phones. You do not need to be registered with Plunket to use this service.
Acknowledgements
Illustration by Dr Greta File. Property of KidsHealth.
References
Tongue tie - information for families | Starship Child Health Newborn Services (PDF, 80 KB)
Tongue tie | Health Info

