Key points about spondylolisthesis in children and young people
- spondylolisthesis is when one bone in the spine slips forward over the bone below it
- it most often affects the bones in the lower back
- many tamariki have mild symptoms or no symptoms at all
- it often develops after a stress fracture in the spine called spondylolysis
- most tamariki improve with rest, activity changes, and physiotherapy
- surgery is rarely needed
What is spondylolisthesis?
The spine is made up of small bones called vertebrae. These spinal bones usually stack neatly on top of each other.
Spondylolisthesis happens when one vertebra slips forward over the one below it. This slip most often occurs in the lower back.
In tamariki and rangatahi (young people), the slip usually happens because of a small stress fracture in part of the vertebra. This part is called the pars. Health professionals may call this a pars fracture.
When this part of the bone has a small crack, it may not hold the vertebra in place as well. Over time, this can allow the bone to move out of position.
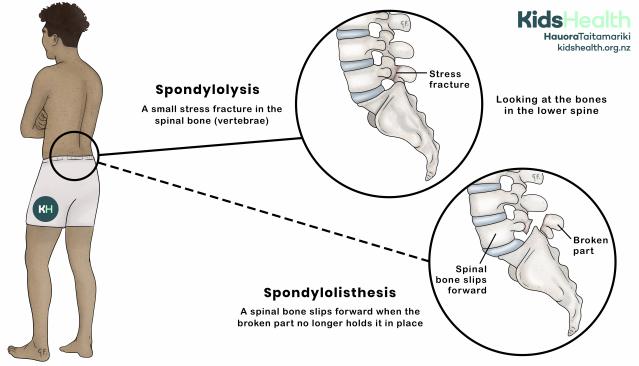
An illustration showing spondylolysis and spondylolisthesis in the lower spine.
Source: KidsHealth
transcribeTranscript
This illustration shows a child’s lower back with close-up views of the lower spine.
- The top circle, labelled Spondylolysis, shows a stress fracture in one of the spinal bones.
- The bottom circle, labelled Spondylolisthesis, shows a broken part of the spinal bone. This allows the spinal bone to slip forward. The illustration highlights the area in the lower spine where these changes occur.
At the top right is the KidsHealth logo with the website: kidshealth.org.nz
A bit about the spine
The spine includes the:
- spine bones (vertebrae)
- intervertebral discs (soft discs between the bones)
- muscles and ligaments that support and move the spine
- the spinal cord and nerves
The vertebrae stack on top of each other to form a strong column. The discs act like shock absorbers. The muscles and ligaments act like strong ropes to hold the bones together and help the spine bend and move.
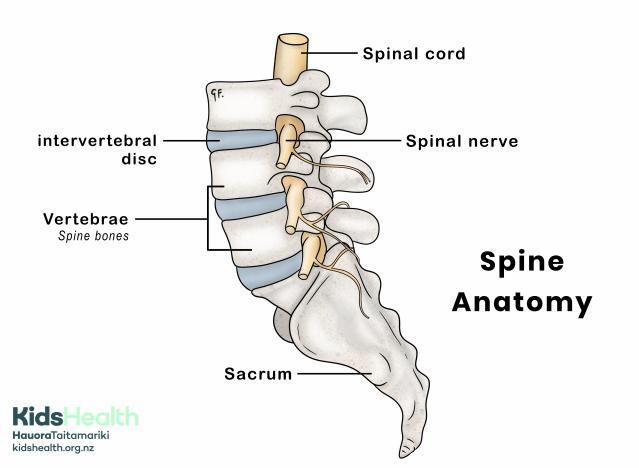
An illustration showing the parts of the lower spine.
Source: KidsHealth
transcribeTranscript
This illustration shows the structure of the lower spine.
- The vertebrae are the bones that make up the spine.
- The intervertebral disc sits between the vertebrae.
- The spinal cord runs down through the spine.
- The spinal nerve branches out from the spinal cord.
- The sacrum is the bone at the base of the spine.
At the bottom left is the KidsHealth logo with the website: kidshealth.org.nz.
Causes of spondylolisthesis
The most common cause of spondylolisthesis in tamariki is a stress fracture in the spine. This stress fracture is called spondylolysis.
Spondylolysis In Children & Young People
Other factors can increase the risk of developing spondylolisthesis, including:
- repeated bending, twisting, or arching of the back
- sports such as gymnastics, football, cricket fast bowling, or diving
- rapid growth during the teenage years
- a history of spinal conditions in the whānau (family)
Symptoms of spondylolisthesis
Some tamariki have no symptoms. Some only find out about the condition after having an X-ray for another reason.
When symptoms do occur, they may include:
- lower back pain that gets worse with activity
- tight hamstrings
- pain that spreads into the buttocks or thighs
- stiffness in the lower back
- changes in posture or walking in more severe cases
Diagnosing spondylolisthesis
A health professional will:
- ask about your child’s symptoms and activity level
- examine your child’s back, posture, and movement
Your health professional may arrange some tests. This may include:
- an x-ray of the spine
- an MRI or CT scan in some cases to check the bones and surrounding structures
Managing spondylolisthesis
Rest
Encourage your child to rest from painful activities and sports. They will need a gradual return to activity once pain settles.
Physiotherapy
Physiotherapy can help improve core strength and flexibility. The physiotherapist can give your child exercises to do.
Pain medicine
Short courses of pain relief medicine may be helpful for flares of pain. Your child shouldn't use pain relief for long periods of time. Talk to a health professional about how long and when to use pain relief.
Paracetamol
If your child has pain, you can give paracetamol to make them more comfortable. You must follow the dosage instructions on the bottle. It is dangerous to give more than the recommended dose.
Other medicine
Your doctor may give your child ibuprofen (such as Nurofen or Fenpaed). You can also buy it at the pharmacy. Follow the dosage instructions carefully. It is dangerous to give more than the recommended dose. Never give your child aspirin. Aspirin can increase the risk of Reye syndrome, which is a rare and serious illness.
Brace
Some tamariki may need a brace for a short time, especially if the pain started suddenly. If your child needs a brace, your health professional will talk with you about this.
Surgery
Most tamariki do not need surgery. Health professionals will only consider surgery if your child's symptoms are:
- severe
- worsening
- not improving with other treatments
Can spondylolisthesis be prevented?
You cannot always prevent spondylolisthesis.
However, your child may lower their risk by:
- avoiding overtraining and allowing time for rest
- warming up before sport
- building core strength and flexibility
- listening to pain and not pushing through it
Looking after your child at home
You can support your child by:
- encouraging rest during painful periods
- helping them follow their physiotherapy programme
- supporting a gradual return to sport
- reassuring them that most tamariki recover well
Let your child know that back pain does not mean permanent damage in most cases.
When to get medical help for your child
When to see a health professional
See a health professional if you child has:
- ongoing or worsening back pain
- pain that stops them from normal activities or sport
- pain that does not improve with rest
When to see a health professional urgently
See a health professional urgently if your child:
- has increasing pain
- develops leg pain, weakness, or numbness
- has trouble walking
When to call 111
Call 111 and ask for urgent medical help if your child:
- suddenly cannot move their legs
- loses control of their bladder or bowels
- has severe back pain after a serious injury
