Key points about bronchiectasis
- bronchiectasis (Bx) is where the airways in the lungs have become damaged and scarred
- mucus gets trapped in pockets in the airway, causing chest infections
- the main symptoms of bronchiectasis are a wet-sounding cough that lasts for weeks or happens often, and repeated chest infections
- once your child has bronchiectasis, they usually have it for life
- picking up and managing bronchiectasis early can improve the scarring
- good care can help your child with bronchiectasis stay well
What is bronchiectasis?
Bronchiectasis is when the airways in the lungs have become damaged and scarred. The airways become widened and mucus gets trapped in pockets within the airway. Having extra mucus in the airways means bacteria and viruses can grow quickly and cause infections.
These infections can cause more damage and scarring to the airways and lungs. Once scarring happens, it usually doesn’t go away. But, good treatment can improve the lungs and prevent more damage. Good treatment is especially important in young tamariki because their lungs are still growing.
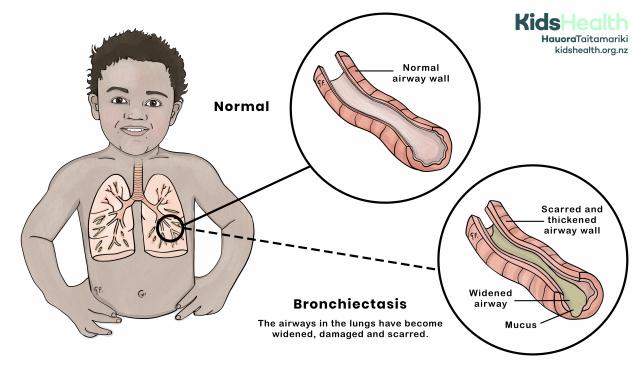
This illustration shows bronchiectasis, where the airways in the lungs become widened, damaged and scarred.
Source: KidsHealth
transcribeTranscript
The image is an anatomical medical illustration designed for educational use, for parents and caregivers of children. It includes the following:
- A young child is illustrated from the waist up, smiling, with both lungs visible on their chest.
- Inside the lungs, bronchi and smaller airways are shown in pale pink with brown and green shading indicating affected areas.
- A circular callout zooms in on a normal airway, labelled 'Normal'. The airway is shown in cross-section, revealing a narrow, smooth interior with uniform walls.
- Another circular callout, connected by a dashed line, zooms in on an airway affected by bronchiectasis. It shows:
- Widened airway
- Scarred and thickened airway wall
- Mucus buildup inside the airway
- A label under the image reads: 'Bronchiectasis - The airways in the lungs have become widened, damaged and scarred.'
- In the top right, the image is branded with the KidsHealth logo and website: kidshealth.org.nz
Causes of bronchiectasis
Common causes
In tamariki, bronchiectasis most often happens after a very bad chest infection or repeated chest infections. Bronchiectasis usually develops after a child has had:
- severe bronchiolitis or pneumonia needing a hospital stay
- chest infections needing repeated antibiotic treatment
- a wet sounding cough lasting for weeks or happening often
Less common causes
Immune system problems
Some tamariki have immune system conditions that make it harder for their body to fight off infections.
Medicines
Some medicines (such as oral steroids) can make it harder for the body to fight off infections.
Objects stuck in the airway
If a child breathes in a small object and this gets stuck in the airway, it can cause a blockage that can lead to scarring. Examples of objects that can get stuck are a nut or a piece of a toy.
Food or liquid going into the lungs (aspiration)
Tamariki who have trouble controlling their swallow will sometimes cough or choke when feeding. Food can end up in their lungs. This can also happen if food refluxes from the stomach and ends up going into the lungs. Over time this can cause bronchiectasis.
Primary ciliary dyskinesia
In primary ciliary dyskinesia, the tiny mucus-clearing hairs (cilia) in the lungs are not working properly. Cilia help move mucus and when they don’t work properly, there is a buildup of mucus in the lungs.
How long bronchiectasis lasts
Once a person has bronchiectasis, they usually have it for life. Good treatment stops it from getting worse and in very young tamariki, can reverse some of the disease.
Signs and symptoms of bronchiectasis
Tamariki with bronchiectasis feel well most of the time.
Wet-sounding cough
A wet-sounding cough is the main symptom of bronchiectasis and usually lasts for weeks. Extra mucus (phlegm or sputum) in the airways causes the cough and your child may spit or cough up some of this mucus.
This cough may be worse during infections, first thing in the morning and during exercise. But, it’s still important for tamariki with bronchiectasis to be active. Exercise and sport help keep them healthy.
When to get medical help for your child with bronchiectasis
When tamariki with bronchiectasis become unwell, they cough more and the mucus can change colour from clear to yellow or dark green. The mucus can sometimes be smelly. They may lose their appetite and feel tired.
When to see a health professional
Call Healthline on 0800 611 116 or see a health professional if your child with bronchiectasis:
- is breathing faster than normal
- has a fever
- has pain in their chest
- is tired and not eating or drinking as well as normal
- is unable to take part in sport and exercise
- has a bad cold
- is coughing more than usual
- has a cough that is wetter than usual
- has more mucus which is darker, thicker or smelly
When to see a health professional urgently
See a health professional urgently if your child with bronchiectasis:
- gets suddenly more unwell
- coughs up blood
When to call 111
Call 111 within New Zealand (use the appropriate emergency number in other countries) for urgent medical help if your child:
- is struggling to breathe is blue around the mouth
- is hard to wake
- is floppy
- is coughing up a large amount of blood
Tests for bronchiectasis
Chest x-ray
Your child’s health professional will arrange a chest x-ray if they think your child may have bronchiectasis. A chest x-ray is usually the first test but it doesn't always show bronchiectasis damage very well. Your child will probably also need a chest CT scan.
CT scan
A CT scan can give a detailed picture of your child’s lungs and can show any scarring or damage of the airways. Chest CT scans show bronchiectasis damage well.
This chest CT scan shows bronchiectasis damage in one lung.
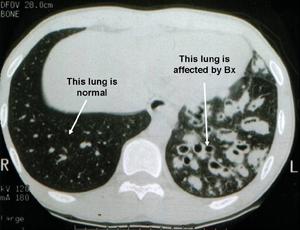
A medical CT scan image of lungs showing a comparison between a normal lung on one side and a lung affected by Bronchiectasis on the other side.
Sputum culture
Your health professional will arrange for your child to get a sample of their mucus (sputum) tested. Many tamariki will be able to cough some mucus into a jar. Sometimes, a physiotherapist might need to help your child collect a mucus sample.
The mucus is tested for bacteria or viruses. If your child's mucus has bacteria, your health professional will give them the right antibiotic to treat the infection.
Blood tests
Your child will have some blood tests to show that they are able to fight off infection.
Lung function test
A lung function test helps to measure how well the lungs are working. This involves your child breathing into a machine. It usually takes about 15 minutes.
Bronchoscopy
A doctor can use a special telescope (bronchoscope) to look into the lungs to see how the airways look and to take a sample of mucus. This test happens while your child is asleep under a general anaesthetic.
Flexible Bronchoscopy In Children
Other tests
Sometimes your child may need other tests, such as a sweat test (to look for cystic fibrosis).
Treatment for bronchiectasis
Chest physiotherapy
Chest physiotherapy helps your child to clear the extra mucus from their lungs. The physiotherapist will show you and your child the best method to use. Your child may need to practice this once or twice a day.
There are different ways to do chest physiotherapy. One way involves breathing and percussion (tapping the chest wall). Other ways involve using physiotherapy breathing devices.
The type of chest physiotherapy tamariki need changes with age.
Exercise and sport
Exercise or playing sport 3 to 4 times a week will help your child to clear mucus from their lungs. It also helps support lung development. Any type of exercise is good, especially if it makes your child take deep breaths. It’s OK if your child coughs during exercise.
Antibiotics
Your child will need antibiotics if they get sick or if they start coughing more. Tamariki with bronchiectasis need a longer course of antibiotics (10 to 14 days). Most often, you can give your child antibiotics at home. Sometimes, if your child is very unwell, they may need antibiotics in hospital.
Asthma treatment
Some tamariki with bronchiectasis can also have asthma. Asthma medicine may help with some of their symptoms.
Bronchiectasis action plan
Tamariki and young people with bronchiectasis may find an action plan helpful. Talk to your child’s health professional to see if it’s right for your child.
The action plan lists your child's daily treatment and steps to take if your child becomes unwell.
Keeping your child with bronchiectasis well
There are several important ways parents and whānau can support their child with bronchiectasis.
Smoke-free and vape-free environment
Keep your child’s environment smoke-free and vape-free. If you want to give up smoking or vaping, contact Quitline or talk with your health professional or whānau.

If you want to give up smoking call Quitline free on 0800 778 778. Quitline can provide free support and advice to help you or someone in your whānau quit smoking. Visit their website for more information.
Healthy balanced diet
Giving your child a healthy, balanced diet helps them to keep well.
Vaccinations
Keep your child’s routine vaccinations up to date. Your child should also get the flu vaccine every year.
Keeping your home warm and dry
Keeping your home warm and dry over winter helps keep your whānau healthy.
Health appointments for bronchiectasis
Outpatient clinics
Your child will have regular reviews with the hospital team. The team can include lots of different health professionals. How often the reviews happen depends on how well your child is.
The reviews will include:
- height and weight measurements to check growth
- lung function tests to measure how well your child's lungs are working
- a mucus sample to test for bacteria so your child can get the right antibiotics
- a cough suction if your child is young and can't cough up mucus
- a check on how you're going with physiotherapy techniques and whether they need changing
A stay in hospital
If your child has a bad chest infection, they may need to go to hospital. Sometimes they need to stay for 10 to 14 days to have specialist treatment and tests.
Antibiotics
While in the hospital, your child may need antibiotics directly into a vein through a 'drip'. Sometimes your child will have a special drip called a 'PICC line'. This is a long tube which lasts for longer than a 'drip' - it doesn't need replacing regularly.
Chest physiotherapy
A professional physiotherapist will do this twice a day.
Tests
Sometimes, your child will have extra testing just like they do at outpatient appointments such as:
- lung function testing
- mucus sampling
- chest x-ray
Cough-free - the way to be video
A long-lasting wet cough can lead to the development of lung diseases such as bronchiectasis. See a video narrated by former Warriors rugby league player Wairangi Koopu. It focuses on knowing the signs of infection that can lead to bronchiectasis. It advises viewers to act on these signs.
Source: Ministry of Health and Health TV
transcribeTranscript
Wairingi Koopu (rugby league star):
Can you hear that? This is the sound of a child with chronic persistent wet cough. Scary, isn’t it? Whānau, this is a serious warning sign and should not be ignored. Your child needs urgent medical attention.
What is chronic persistent wet cough?
Dr Cass Byrnes (paediatric respiratory specialist, Starship Hospital):
A chronic persistent wet cough is a mucousy phlegmy fruity-sounding cough. It sounds like the children have got mucus down in their chest and it usually occurs most days and can go on for weeks at a time.
Here is an example.
This cough is not normal and may be a sign that your child has a serious chest infection. It is important that your child sees a doctor as they could develop a serious lung disease.
What happens if chronic persistent wet cough is not treated?
If a chronic persistent wet cough is not treated it can go on for weeks and even months, and it’s a sign that there’s an ongoing chest infection in the lungs and it essentially is causing some permanent scarring in the lungs.
Wairingi Koopu:
Chronic persistent wet cough if left untreated can lead to lung damage and disease such as bronchiectasis.
What is bronchiectasis?
Bronchiectasis is a chest disease in which the breathing tubes called bronchi in the lungs become damaged and enlarged. Tiny hairs called cilia line the inside of these breathing tubes. These hairs help to collect any phlegm or mucus from the lungs.
When your child has bronchiectasis their lungs make more mucus than normal. The tiny hairs that should clear the mucus stop working properly and the mucus gets stuck in the breathing tubes. It is within this extra mucus that germs grow and cause infection.
These infections cause damage and scarring to the breathing tubes and lungs. The breathing tubes become baggy and holes form in the lungs. Once this has happened the scarring and damage cannot be fixed.
What causes bronchiectasis?
Dr Cass Byrnes:
Bronchiectasis is a type of permanent lung scarring which is caused by having ongoing infection in your lungs. That mucus means that there’s mucus and bugs down there and it’s breaking up some of the lung walls and doing lung damage.
What are the symptoms of bronchiectasis?
Wairingi Koopu:
Children with bronchiectasis will feel well most of the time but the main symptom to look out for is the chronic persistent wet cough. This cough produces a build-up of phlegm which may be yellow or green in colour and smelly, showing signs of infection. It is important that you seek medical attention if your child has these symptoms.
What happens if we ignore this symptom?
Dr Cass Byrnes:
Ignoring the chronic persistent wet cough means that you’re going to go on and develop more and more lung scarring. That cough shows that there are problems in the lung. It shows that there is a build-up of mucus, that there is infection and the more and longer that that goes on, the more damage that that lung is going to have permanently lifelong, and set the child up for recurrent further infections.
How can bronchiectasis be prevented?
Wairingi Koopu:
By:
not smoking during pregnancy
breastfeeding our tamariki
early detection and treatment of chest infections in childhood
improving living conditions
eating a healthy balanced diet
immunisation.
We visit the Hiko whānau who deal daily with the effects of having tamariki with bronchiectasis.
Henrietta Hiko (mother of twins):
The illness has changed our lives immensely. I have to give up everything pretty much to go back and forth to the hospital when the girls are sick. They’re sick at the moment but they don’t look it, but I know that they’re sick.
How can a parent manage bronchiectasis? What can they do?
Kimberley Taylor (physiotherapist, Hawkes Bay District Health Board):
Some easy ways that parents can help to manage their tamariki’s bronchiectasis are to get them more active. Exercising outside, running around, on the trampoline, anything that makes them huff and puff, because when you’re huffing and puffing you’re getting air circulating all the way down to the bottom of your lungs and that helps to shift the mucus.
Other things that are really good to help with managing bronchiectasis are to keep your whare auahi kore – so keeping your tamariki smoke-free and telling your whānau to keep outside of the whare when they’re smoking and out of the waka when they’re smoking.
Wairingi Koopu:
If you are concerned about your child's health, please seek medical attention.
For more information please visit the Asthma Foundation website.
Support and more information about bronchiectasis

The New Zealand Bronchiectasis Foundation website has a range of resources and information.
Acknowledgements
Illustrations by Dr Greta File. Property of KidsHealth.
Starship Foundation and the Paediatric Society of New Zealand acknowledge the cooperation of the Starship Respiratory Service at Starship Children's Health and the Paediatric Department, University of Auckland in making this content available to patients and families.
