Bronchiolitis animation
Find out what bronchiolitis is and what to do if your child gets bronchiolitis.
Source: KidsHealth
transcribeTranscript
Bronchiolitis is a common illness that’s very easy to catch.
Bronchiolitis usually affects pēpi under the age of one.
Bronchiolitis usually starts as a cold.
Pēpi with bronchiolitis:
- cough
- breathe harder and faster
- have noisy breathing
- and may have a fever
Symptoms can last for several days.
Bronchiolitis is usually a mild illness.
You can expect your baby to get completely better.
Some pēpi may need to go to hospital if they need oxygen or can't feed.
See a health professional urgently if your baby has any of the following:
- is under 3 months old or
- is breathing fast, has noisy breathing or is working harder to breathe or
- looks unwell or
- is taking less than half of their normal feeds or
- is vomiting
If you are worried, call Healthline on 0800 611 116 or go back to a health professional.
Dial 111 if your baby:
- is blue around the mouth or
- is struggling to breathe or
- is hard to wake or
- is floppy
Bronchiolitis animation in te reo Māori.
Source: KidsHealth
transcribeTranscript
Ko te mate pekahau ririki he mate e kitea whānuitia ana, he mate tino hopuhopu nei hoki.
He rite tonu te pā mai a te mate pekahau ririki ki ngā pēpi kāore anō kia tae atu ki te kotahi tau te pakeke.
He rite tonu te tīmatatanga o te mate pekahau ririki ki te maremare noa.
Ko ngā pēpi kua pāngia mai e te mate pekahau ririki:
- ka mare
- ka kaha ake, ka tere ake hoki te hēhē
- ka hoihoi te hēhē
- ka kirikā pea
Ka noho pea ngā tohumate mō ētahi rā.
I te nuinga o te wā ko te mate pekahau ririki he māuiui māmā.
Ko te matapae ka piki katoa te ora o tō pēpi.
Ko ētahi pēpi, me haere pea ki te hōhipera ki te hiahia hāora rātou, ki te kore rānei rātou e taea te whāngai atu.
Kia kōhukihuki tō toronga atu ki tētahi ngaio hauora mēnā:
- kāore anō kia tae atu ki te 3 marama te pakeke o tō pēpi tērā rānei
- e tere ana te hēhē, kua hoihoi te hēhē, ka uaua ake rānei te hēhē o tō pēpi tērā rānei
- e māuiui ana te āhua o tō pēpi tērā rānei
- e kai ana tō pēpi kia iti iho i te haurua o āna kai māori tērā rānei
- e ruaki ana tō pēpi
Mēnā he āwangawanga āu, waea atu ki Healthline ki 0800 611 116 hoki atu rānei ki tētahi ngaio hauora.
Waea atu ki 111 mēnā:
- he kikorangi te taha o te waha o tō pēpi tērā rānei
- kei te hēmanawa tō pēpi tērā rānei
- he uaua te whakaoho i tō pēpi tērā rānei
- he pītawitawi tō pēpi
Bronchiolitis animation in Samoan.
Source: KidsHealth
transcribeTranscript
O se faamai taatele ma pepesi gofie.
E masani ona aafia ai pepe e le i atoa le tasi tausaga o le matua.
E amata mai i le fulū.
O pepe ua maua ai:
- tale
- taumafai malosi ma televave le mānava
- taagulugulu le mānava
- e ono maua i le fiva
E faitau aso o maua ai i āuga.
E le o se faamai e tigaina ai.
E tatau ona toe foi i le manuia si au tama.
E iai pepe e ono moomia le ave i le falemai pe a moomia se okesene po o le lē mafai ona fafaga.
Vaai loa se sui faalesoifua maloloina pe afai o si au tama:
- e le i atoa le 3 masina po o le
- televave lana mānava, taagulugulu le mānava po o le taumafai malosi e mānava po o le
- foliga ma'i po o le
- lē ‘afa le telē o se meaai o mafai na ‘ai po o le
- faasuati
Afai o e popole, vili le Healthline i le 0800 611 116 po o le toe vaai le sui faalesoifua maloloina.
Vili le 111 pe a vaaia tulaga nei i si au tama:
- lanu moana le gutu po o le
- tau mānava po o le
- tau fafagu po o le
- faapalupē
Bronchiolitis animation in Tongan.
Source: KidsHealth
transcribeTranscript
Ko ha mahaki angamaheni ‘a e bronchiolitis ‘oku faingofua ‘aupito ke puke mei ai.
‘Oku fa‘a uesia ‘e he bronchiolitis ‘a e fanga ki‘i pēpē si‘i hifo ‘i he ta‘u tahá.
‘Oku fa‘a kamata ‘a e bronchiolitis ‘aki hano ma‘u ‘e he momokó (cold).
Ko e fanga ki‘i pēpē ‘oku puke ‘i he bronchiolitis ‘oku:
- nau tale
- faingata‘a mo vave ange ‘enau mānavá
- longolongoa‘a ‘enau mānavá
- malava kenau mofi
‘E lava ke ‘asi ‘a e ngaahi faka‘ilonga ‘o e mahakí ‘i ha ngaahi ‘aho lahi.
‘Oku fa‘a tō ma‘ama‘a pē ‘a e bronchiolitis.
‘E lava ke ke ‘amanaki atu ‘e sai pē ‘a e puke ho‘o pēpeé ‘o mo‘ui lelei.
‘E ala fiema‘u ke ‘ave ha fanga ki‘i pēpē ‘e ni‘ihi ki falemahaki kapau tenau fiema‘u ha ‘osikena (oxygen) pe ‘ikai lava ‘o kai.
Sio leva ki ha tokotaha ngāue palofesinale ki he mo‘ui leleí ‘i he vave tahá kapau ko ho‘o pēpeé ‘oku:
- si‘i hifo ‘i he māhina ‘e 3 hono ta‘u motu‘á pe
- vave ‘ene mānavá, longolongoa‘a ‘ene mānavá pe faingata‘a ange ‘ene mānavá pe
- mata‘i puke pe
- si‘isi‘i ange ‘i he vaeuá ‘a e lahi ‘o e me‘akai angamaheni ‘oku ne kaí pe
- lua
Kapau ‘okú ke hoha‘a, telefoni ki he Healthline ‘i he fika 0800 611 116 pe toe foki ki ha tokotaha ngāue palofesinale ki he mo‘ui leleí.
Taila ‘a e 111 kapau ko ho‘o pēpeé ‘oku:
- lanu pulū takatakai ‘a e ngutú pe
- faingata‘a‘ia ‘ene mānavá pe
- faingata‘a ke ‘ā‘ā pe
- tāvaivaia
Watch an animation on bronchiolitis in your preferred language.
Key points about bronchiolitis
- bronchiolitis causes breathing problems in pēpi
- bronchiolitis is very easy to catch
- breastfeeding and a smoke-free environment give the best protection against bronchiolitis
- bronchiolitis is usually a mild illness but some sicker pēpi need to go to hospital
- there is no medicine that makes bronchiolitis better
- if your baby with bronchiolitis is under 3 months old, you should always see a health professional
What is bronchiolitis?
Bronchiolitis is a common illness usually caused by a virus. The most common are RSV (respiratory syncytial virus) and rhinovirus but there are many viruses that can cause bronchiolitis.
Respiratory Syncytial Virus (RSV) Infection
Bronchiolitis affects the smallest airways (called bronchioles) throughout the lungs.
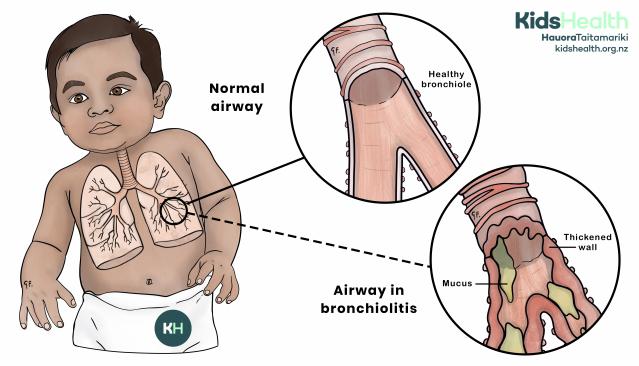
This illustration shows bronchiolitis, where the airways in the lungs become swollen and filled with mucus compared with a normal airway.
Source: KidsHealth
transcribeTranscript
The illustration shows a young child with an overlay of the lungs and windpipe on their chest. A circle highlights the bronchioles, with two enlarged diagrams comparing normal and bronchiolitis.
- The top circle is labelled Normal airway. It shows a healthy bronchiole with a clear passage. The label reads: Healthy bronchiole.
- The bottom circle is labelled Airway in bronchiolitis. It shows a bronchiole with a thickened wall and mucus blocking the airway. The thickened wall and mucus are labelled.
At the top right is the KidsHealth logo with the website: kidshealth.org.nz
Catching bronchiolitis
Bronchiolitis is very easy to catch - it can spread easily.
It is most common in winter and spring.
Who gets bronchiolitis
- bronchiolitis usually affects pēpi under the age of one
- pēpi who are around people who smoke or vape are more likely to get bronchiolitis
- severe bronchiolitis is more common in premature pēpi or pēpi with heart or lung problems
A paediatrician may recommend a medicine to prevent serious illness caused by RSV in high-risk babies. (RSV is a common cause of bronchiolitis).
RSV Passive Immunisation For High Risk Babies
Signs and symptoms of bronchiolitis
Bronchiolitis often starts as a cold, with a runny nose.
Pēpi with bronchiolitis:
- cough
- breathe harder and faster
- have noisy breathing (wheeze)
- may have a fever
The second or third day of the chesty part of the illness is usually the worst.
Bronchiolitis can last for several days. The cough often lasts for 10 to 14 days but it may last as long as a month.
Watch this video of a baby with noisy breathing (wheezing)
Damian Roland's YouTube channel
When to get medical help for bronchiolitis
When to see a health professional urgently
See a health professional urgently if your baby:
- is under 3 months old
- is breathing fast, has noisy breathing and is working harder to breathe
- looks unwell
- is taking less than half of their normal feeds
- is vomiting
- has not had a wet nappy for more than 6 hours
Signs That Children Are Struggling To Breathe
See a health professional or call Healthline (0800 611 116) if you are worried about your baby.
When to call 111
Call 111 within New Zealand (use the appropriate emergency number in other countries) and ask for urgent medical help if your baby:
- has blue lips and tongue
- has severe difficulty breathing
- is becoming very sleepy and not easy to wake up
- is very pale
- is floppy
- has breathing that is not regular, or pauses in breathing
Treatment for bronchiolitis
Most babies get better by themselves
Most pēpi with bronchiolitis get better by themselves without any special medical treatment.
- antibiotics do not help pēpi with bronchiolitis because it's caused by a virus
- asthma puffers or inhalers don't help pēpi with bronchiolitis
- using reliever asthma puffers or inhalers in pēpi less than 12 months of age may make their breathing worse
- steroid medicine by mouth or inhaler does not help pēpi with bronchiolitis
- in pēpi over 12 months of age, it may be hard to tell if the problem is bronchiolitis or viral wheeze - your health professional may try asthma puffers or inhalers
Babies with more serious illness may need to go to hospital
Pēpi with more serious bronchiolitis may need to go to hospital. Sometimes pēpi need help with their breathing. This might include extra oxygen through small soft plastic tubes that fit into your baby's nose.
If your baby is not feeding enough, they may need:
- feeding through a nasogastric tube (a tube that goes up the nose and down into the stomach)
- fluids through an intravenous drip (a tube into a vein)
Caring for your baby with bronchiolitis at home
Babies who can stay at home
- pēpi who are feeding well
- pēpi who do not look sick
- pēpi who are not working too hard with their breathing
Suggestions for looking after your baby
Pēpi with bronchiolitis may not be able to feed for as long as usual. Offer smaller feeds more often.
Give your baby as much rest as possible.
Don't smoke in the house or around your baby.
Keep your baby's nose clear. If it is blocked or crusty you can use saline nose drops (from a pharmacy).
Keep your baby away from other pēpi and tamariki, and from childcare centres, to stop bronchiolitis spreading.
If your baby is miserable and upset, you can give paracetamol. You must follow the dosage instructions on the bottle. It is dangerous to give more than the recommended dose.
Preventing bronchiolitis
Breastfeeding
Breastfeeding pēpi protects them from getting bronchiolitis by boosting their infection-fighting (immune) system. Breastfeeding beyond 4 months of age offers the best protection.
Smoke-free environment
Make sure your baby's environment is smoke-free. If you want to give up smoking or vaping, contact Quitline or talk with your health professional.

If you want to give up smoking call the free Quitline Me Mutu on 0800 778 778 or text 4006. You can find more information on their website.
A warm house
Keeping the house warm and well-insulated will also decrease your baby's risk of developing bronchiolitis.
Stay away from people with coughs and colds
It is sensible to keep young pēpi away from people who have colds and coughs.
Clean hands
Make sure everyone in your family washes their hands regularly and thoroughly and dries them well, including (but not only) before preparing food and eating. This can reduce the spread of infection.
Bronchiolitis is not the same as asthma
Bronchiolitis is not the same as asthma. Most pēpi with bronchiolitis do not go on to have asthma. Asthma is more likely in tamariki if there are other family members with asthma.
Acknowledgements
Illustrations by Dr Greta File. Property of KidsHealth.
